Should we combine lens extraction with filtering surgery?

Combining lens extraction with MIGS/ECP

‘PEcK’ing order in advanced glaucoma
Current gold standard surgical management of advanced glaucoma is trabeculectomy, which is beset with unique sight threatening problems. This video deals with combination of MIGS in advanced glaucoma – can it be safer but as efficacious as trab?
Presenting author: Dr. Surinder Singh Pandav Co-authors: Dr. Srishti Aggarwal Dr. Faisal TT Dr. Manik Manik

‘A sticky situation’ – vitreous occlusion of tube of a glaucoma drainage implant
Spontaneous vitreous occlusion of the tube can occur at any point many years later, despite initial core pars plana or anterior vitrectomy in an aphakic. Surgical removal of the wick by this technique is more effective to ensure tube patency compared to laser treatment alone. In idiopathic cases we may need to consider external triggers for delayed presentation of tube occlusion, such as patient lifestyle and unintentional valsalva maneuvres.

Your WGA
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login
Your Profile
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login
Your Dashboard
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login
You are what you eat: diet and glaucoma

You are so superficial: non penetrating surgery

XX Symposium of the Brazilian Glaucoma Society
Join the XX Symposium of the Brazilian Glaucoma Society! The symposium will take place from March 9-11, 2023, at Convention Armação, Porto de Galinhas.
For more information please visit their website: https://sisbrag.com.br/
XVIII SEG Congress
XVIII Congress of the Spanish Society of Glaucoma
Join the 18th Congress of the Spanish Society of Glaucoma!
The meeting will take place from March 07-09, 2024, in Sevilla, Spain.
For more information visit their website: https://www.sociedadglaucoma.com/18-congreso-de-la-sociedad-espanola-de-glaucoma/
XIX Russian Glaucoma Society (RGS) and Commonwealth of Independent States Glaucoma Society (CIS) Hybrid Annual Meeting
Including XXXIII RGS Advisory Board Meeting, 4th East-Europe Non-Formal Glaucoma Online-Club, and XXI Scientific Vanguard Club. (19+ President Friends!)
Join the Russian Glaucoma Society (RGS) and the Commonwealth of Independent States Glaucoma Society (CIS) for their Annual Meeting which will take place from December 3-4, 2021.
This meeting will take place as a hybrid meeting with both onsite and virtual elements.
For more information visit: http://www.glaucomanews.ru/.

XIII Congress of the Czech Glaucoma Society
Join the Congress of the Czech Glaucoma Society!
The meeting will take place from April 4-6, 2024 in ALDIS Congress Center, Hradec Králové.
For more information visit their website: www.glaukom2024.cz
XEN vs Preserflo

XEN in closed angle glaucoma

XEN Gel Stent Implantation in Primary Open-Angle Glaucoma Patients: Comparison of Surgical Approaches

XEN 45 Safety and outcomes

WSPOS World Wide Connect
World Society of Paediatric Ophthalmology and Strabismus
We at WSPOS believe that with every challenge comes opportunity and the current situation has challenged us to deliver a global conference to a global audience via a virtual platform. So join us on Saturday 26th September for WSPOS World Wide Connect – “Give Us 24 Hours and We’ll Give You the World”
For more information visit: https://www.wspos.org/world-wide-connect-2020/

Wound Healing

World Sight Day 2023
World Sight Day is taking place on Thursday, October 12, 2023, and is focussing the world’s attention on the importance of eye care.
We are calling on the sector to join us to help people prioritize their own eye health and leaders to ensure eye care is accessible, inclusive and affordable to everyone, everywhere.
For more information visit the IAPB website: World Sight Day 2023 – The International Agency for the Prevention of Blindness (iapb.org)
World Sight Day 2022
World Sight Day is taking place on Thursday, October 13, 2022, and is focussing the world’s attention on the importance of eye care.
We are calling on the sector to join us to help people prioritize their own eye health and leaders to ensure eye care is accessible, inclusive and affordable to everyone, everywhere.
For more information visit the IAPB website: World Sight Day 2022 – The International Agency for the Prevention of Blindness (iapb.org)
World Patient Safety Day 2023
World Patient Safety Day is taking place on Sunday, September 17, 2023, and is focussing on patient and family engagement to advance safety in healthcare.
For more information visit the WHO website: World Patient Safety Day 2023 – World Health Organization
World Ophthalmology Congress 2024
International Council of Ophthalmology World Ophthalmology Congress 2024
Join the ICO World Ophthalmology Congress!
The congress will take place from August 16-19,2024, in Vancouver, Canada.
For more information visit their website: https://icoph.org/world-ophthalmology-congress/
World Glaucoma Week 2024
Save the Date!
Join the 2024 World Glaucoma Week from March 10-16,2024.
The theme for this year is Uniting for a Glaucoma-Free World. Let’s join forces in raising awareness on Glaucoma.
Submit your activity here!
World Glaucoma Week 2022
World Glaucoma Week (WGW) is a global initiative of the World Glaucoma Association (WGA) in order to raise awareness on glaucoma. Through a series of engaging worldwide activities, patients, eye-care providers, health officials, and the general public are invited to contribute to sight preservation. The goal is to alert everyone to have regular eye (and optic nerve) checks in order to detect glaucoma as early as possible. In 2022, the WGW will take place between March 6-12.
For more information, visit https://www.worldglaucomaweek.org/.
World Glaucoma Week
“World Glaucoma Week is a global initiative organized by the World Glaucoma Association. We invite patients, eye care providers, health officials and the public to join forces in organizing awareness activities worldwide.
Glaucoma is the leading cause of preventable blindness, and distinct challenges may be present in different regions of the world. Our goal is to alert everyone to have regular eye and optic nerve checks to detect glaucoma as early as possible because there are available treatments for all forms of glaucoma to prevent visual loss.”
World Glaucoma Association
Glaucoma Awareness Slide Deck
Facts about Glaucoma
How Glaucoma may affect your vision?
Get involved
-
-
- Involve your glaucoma patients as you organize a screening event in your local institute/hospital
- Give a lecture to a patient support group
- Participate in radio & TV shows to talk about glaucoma and to answer questions
- Contact newspapers to publish information about glaucoma
- Run a social media campaign
-
More details about World Glaucoma Week and many examples of glaucoma awareness activities around the world are to be found on the WGW website.
World Glaucoma Week
The world is bright, save your sight!
World Glaucoma Week is a global initiative of the World Glaucoma Association (WGA) in order to raise awareness on glaucoma.
The 2021 theme reflects the hope that with regular testing, people continue to see the world around us: full of beauty, charm, and adventure. The world is bright, save your sight!
For more information visit: https://www.worldglaucomaweek.org/
World Glaucoma Congress 2025
Save the date for the 11th World Glaucoma Congress, taking place June 25-28, 2025, in Honolulu, Hawaii, USA!
World Glaucoma Congress
World Glaucoma Association | Home
WOC 2022
World Ophthalmology Congress
The International Council of Ophthalmology will be hosting the 2022 World Ophthalmology Congress on 9-12 September 2022.
For more information visit: https://icowoc.org/congress-information/
WOC 2020
Join WOC2020 Virtual®
The ICO is excited to bring the world congress to each of you in the form of a virtual experience – WOC2020 Virtual®, 26–29 June 2020. This first of a kind World Ophthalmology Congress experience will showcase world-class scientific program with over 2,000 presentations from leaders and experts from 181 ICO member societies.
WOC2020 Virtual® offers interactive networking opportunities with live streaming features that will include our committed corporate partners, with industry symposia and more. The virtual experience will be more accessible than ever before with an opportunity to come together, collaborate and share the latest advancements in eye care.
Join WOC2020 Virtual® for innovative, unique, and dynamic learning opportunities from the comfort of your own home and earn CME points.
Register now to access over 2.000 presentations, +100 live sessions including live Q&A and interactive polls, 250 recorded sessions, and much more. All content will be available on-demand for 3 months after the congress.

With recent advances in optic nerve imaging, I believe that baseline optic nerve stereo photos are still essential
Most important to patients is their feeling and functioning. It is easy to be mislead by central corneal thickness, intraocular pressure , and cup/disc ratios, which do not relate to feeling and function at all, visual fields, often invalid and noisy, and retinal nerve fiber layer thickness, which is affected by many conditions other than glaucoma, including myopia. The appearance of the optic disc is most closely related to diagnosis and severity; photographs provide the best way to monitor change
From the Education Committee
Despite the difficulties related to learning glaucomatous optic disc patterns, optic disc evaluation and high quality photos are still the most valid and relevant method for diagnostic and follow-up purposes, according to Professor George Spaeth. Access this video to understand why.

With recent advances in optic nerve imaging, I believe that baseline optic nerve stereo photos are now unnecessary
In contrast to George Spaeth, Felipe Medeiros was asked to explain why stereo photos are now unnecessary. From the difficulties related to how to evaluate digital photos, to the lack of quantitative assessment of rates of change, this lecture provides more information on this topic.

Will MIGS replace non-penetrating surgery?
Dr. Alain Bron pointed out the idea that there is a good surgery for the patient and a good surgery for the surgeon and our task is to make a mixture. He discussed the problems with non-penetrating surgery leading to its relative unpopularity and compared them to the problems with MIGS. He expressed the view that new evolving techniques will help us to understand how glaucoma surgery works.

Will cell-based strategies be realistic for glaucoma treatment?

Wide field scan imaging with swept-source OCT for glaucoma diagnosis
Advantages of wide-field map of posterior pole analysis:
1. Has the information needed to diagnose early glaucoma with excellent sensitivity/specificity.
* Optic nerve head + macula in a single scan
* Capability to segment both mGCIPL and cpRNFL
2. Minimizes problems with alignment if comparing macular and circumpapillary data.
* RNFL defects apart from the optic disc can be more easily visualized
* More sensitive in visualizing the temporal margin of RNFL defect.
* The potential to improve our understanding of the relationship between optic nerve and macular damage

Why would you even bother mapping genes? Translation of GWAS results
Dr. Stuart MacGregor talked about translation of Genome-Wide Association Studies results and why would we need genes mapping. He discussed causal Inference, new drug targets, genetic risk prediction examples. He stated that GWAS has identified many glaucoma risk loci, is useful for causal inference. It helps identifying new drug targets. He talked about genetic risk prediction and mentioned that good risk stratification in general population may help identifying disease progression in early disease or need for surgery in advanced disease.

Why trabeculectomy is still important

Why operate , just use Lasers (SLT/ Micropulse)

Why Does IOP Vary

Why Does IOP Fluctuate?
This content is restricted and only accessible to WGC-2019 participants
Login

Why do we need OCT in a glaucoma clinic ?

Why do ganglion cells die? Is this a key to cure or prevention?
Clinical trials of new therapies to prevent neurodegeration in glaucoma remain an important goal.

Why do ganglion cells die in glaucoma

Why did I get glaucoma with a normal pressure? Answering the question for your patient

Who should be treated?

Who said glaucoma is an incurable disease?
Effective “cure” requires protection / repair of all compartments of RGC
Multiple strategies now exist that show promise
Clinical trials are possible and achievable . . .
Combinations of treatment may be required for maximum benefit
“Protect and regenerate” could be the future . . . ?
From the Education Committee
Dr. Keith Martin addresses recent studies suggesting that neuroprotection and neuroregeneration is possible in glaucoma and may translate into novel therapies in the future. He summarizes by suggesting how clinical trials based on pressure-independent therapies are possible and the need for combining different approaches to cure glaucoma.

Who is going to get worse? Cutting-edge methods for predicting disease progression

Which patients don’t need our help?
Which MIGS to choose for which patient?

Which Angle Closure Eyes require a Laser Iridotomy? | Benjamin Xu
This video describes current evidence regarding the role of laser peripheral iridotomy (LPI) in patients with angle closure.
In brief, both the World Glaucoma Association (WGA) and American Academy of Ophthalmology (AAO) recommend that patients with primary angle closure (PAC) or primary angle closure glaucoma (PACG) should receive LPI treatment unless they are candidates for lens extraction surgery.
Guidelines for primary angle closure suspects (PACS) are less clear. Fellow eyes of acute primary angle closure (APAC) eyes should receive prophylactic LPI due to high risk of APAC. PACS patients who require frequent dilation, are older, or have severe angle narrowing on OCT imaging may also benefit from prophylactic LPI.

Which angle closure eyes benefit from lens removal/cataract surgery? | Augusto Azuara-Blanco
This video describes current evidence regarding the role of lens extraction in patients with angle closure.
In brief, patients with co-existing angle closure and cataract will benefit from early lens extraction. For those patients with clear lens and significant angle closure disease there is evidence that phacoemulsification is more effective than peripheral laser iridotomy.
Combining cataract and glaucoma surgery (e.g., trabeculectomy) may be more effective than phaco alone, and could be considered in patients with severe glaucoma, but there are uncertainties and combined surgery may be associated with an increased risk of complications.
At the moment it is not possible to identify or predict what ocular characteristics help predict a better outcomes after surgical and laser interventions.

Where tubes fit in

When to use laser

When to use and which implant to use?

When to perform a clear lens extraction: Risks versus benefits

When to go for Surgical Intervention?

When things look Bleak ,there is always a silver lining. The Quadruple procedure in Microspherophakia
The video illustrates the benefits of quadruple procedure (GDD,PPV,PPL,SFIOL) in a microspherophakic eye with gross lens subluxation and advanced glaucoma at risk of progression & loss of central vision.
Sharmila Rajendrababu-Consultant,Aravind eye care system,Madurai Mythri Rao -Glaucoma fellow ,Aravind eye care system,Madurai Palanikumar-Audiovisual consultant,Aravind eye care system,Madurai

When should I initiate a treatment in Glaucoma suspects?

When it’s not glaucoma: The neuro-ophthalmologic differential diagnosis

When is phaco trab the best procedure with open angles?
Pahcoemulsification alone results in a modest IOP reduction in POAG patients, whie phacomeulsification + MIGS provides additional IOP lowering, which can be advantageous in eyes with early to moderate POAG. Eyes with advanced POAG and eyes that do not tolerate medications benefit from a combined phacoemulsification + trabeculectomy.
From the Education Committee
Dr. Costa compared the surgical options available for open angle glaucoma: Phaco alone/Phaco+MIGS/Phaco+Trab. He said while Phaco and MIGS bring about only a modest IOP reduction, Phaco+Trab may be preferred in cases with advanced glaucoma where target IOP is in low teens or the patient is non-compliant to anti-glaucoma medications.

When is phaco alone the best procedure with open angles?
The higher the pre-op IOP the greater the IOP reduction, postoperative effects appear to last at least 2 years and potentially longer than 4 years, however post-op IOP spikes of significant magnitude happen
From the Education Committee
Dr. Jinapriya did an elaborate review of literature and suggested that higher the preoperative IOP, higher is the postoperative IOP reduction after cataract surgery. This IOP lowering effect was seen to last between 2-4years. He concluded by enumerating the scenarios where phaco alone is the best procedure in open angle glaucoma: medically controlled, preoperative IOP and postoperative target IOP in mid teens, optic nerve could sustain IOP spike after cataract surgery and compliance with medications is not a problem.

When is phaco alone not enough for PACD?

When is my patient safe to drive (or not)?

When is laser iridotomy indicated in primary angle closure glaucoma suspects?

When I do trab and when I do tube?
Primary tube versus primary trab:
Trabe has a higher success rate compared to tube
Rate of reoperations and intraoperative complications is similar in both groups
Less medications in trab
trab is cheap, tube expensive.
no foreign body in trab
From the Education Committee
Dr. Esther Hoffman discussed difficult choices and started with the main points for the surgeon first of all to be right in your diagnosis, to be sure if this is really glaucoma. She also described the results of clinical studies proving that both methods are effective in IOP lowering, no clear superiority, but tube shunt surgery showed lower failure rates. Surgeon’s skills and experience are important factors. She provided her personal decisions for trab or tube.

When I do trab and when I do MIGS?
1.- Trabecular MIGS and Conventional Filtering Surg have different indications.
2.- MIGS PLUS/MPEGS and Conventional Filtering Surg overlap. New options are less aggressive (Flaps, bleeding…),more reproducible and have fewer complications.
– However, the should also consider the added cost and no long term data are available (IOP and safety).
– Postop care is crucial to improve the success rate of these bleb-dependant surgeries. (Needling, bleb revision…).
3.- In our indications we should consider patient profile and expectations.
From the Education Committee
Dr. Julian Garcia Feijoo discussed the role for MIGS devices and Trab based on the clinical experience and existing scientific evidence. The target IOP range, stage of disease, rate of progression, age, topical treatment regime, number of drops are different among glaucoma patients. Surgeon’s choices are affecting patient’s quality of life. Patients have expectations for safe surgery, low complication rate, efficacy. He suggested to think about ocular features, type of glaucoma, patient’s life expectancy. Safer surgeries are not risk free surgeries.

When glaucoma is not so straightforward – case presentations

When do I get anterior segment imaging done?

When can I trust this visual field?
We are honored to have Pradeep Ramulu MD, PhD, Chief of the Glaucoma Division and Professor of Ophthalmology at the Wilmer Eye Institute at Johns Hopkins Hospital, USA, present this webinar.
Dr. Ramulu grew up in suburban Chicago and became interested in the eye during medical school, during which time he studied the genes and proteins of the eye with Dr. Jeremy Nathans. After pursuing a residency in ophthalmology and fellowship training in glaucoma, he joined the Wilmer glaucoma faculty in 2006, where he specializes in caring for both routine and complex glaucomas, including glaucomas requiring repeat operations, glaucoma occurring in the context of corneal or retinal disease and glaucoma occurring in newborns and young children.
Dr. Ramulu’s research focuses primarily on how glaucoma affects the individual. Specifically, he has studied the types of difficulties that glaucoma patients experience with regards to reading, walking, falling, driving and traveling outside the home. His long-term interests are to understand when and how glaucoma should be treated based on a more complete understanding of how patients are affected by their disease. Additionally, his work is geared toward developing rehabilitative strategies for individuals with severe vision loss from glaucoma and in developing recommendations to increase the safety and quality of life of all individuals with glaucoma.
Topic: When can I trust this visual field?
This webinar started with an introductory presentation on the topic by Pradeep Ramulu MD, PhD, followed by an online group discussion with all attending as well as a Q&A with Dr. Ramulu.
Is it for me?
We welcome all ophthalmologists and other healthcare professionals related to glaucoma to watch this webinar. Whether you have 2 or 20 years of experience, this webinar is designed to accommodate eye care providers and glaucoma specialists at every stage in their career.
What will I learn?
- Latest insights on when to trust a visual field
- Exchange thoughts and knowledge on the topic with your peers from every corner of the world
- Exclusive opportunity for a Q&A with Dr. Ramulu

When and how to needling after Trabe

When and how to do Cyclophotocoagulation in seeing eyes

What’s great about the World Glaucoma Congress?
A unique opportunity for glaucoma specialists and related health care professionals to come together and contribute to the exchange of glaucoma knowledge. Learn more about the World Glaucoma Congress in this short video.
At the World Glaucoma Congress 2019 in Melbourne Australia, host Josh Szeps sat down with Keith Martin (President WGA 2017-2019), Anne Brooks (President ANZGS), Shan Lin (Executive Vice President WGA) and Kaweh Mansouri (Associate Executive Vice President WGA) to talk about the World Glaucoma Association.

What visual field testing strategy should I use? (SITA Standard/Fast/Faster 30-2/24-2/24-2C) | Anders Heijl
This video will discuss choosing SITA tests for glaucoma management. Original SITA Standard and SITA Fast strategies represented a change of paradigms: time-saving, very computer-intensive with maximum likelihood estimations in real time. SITA Faster is a further development of SITA Fast. Definitively detecting perimetric progression and measuring rate of progression usually requireat least 5 tests. Making this possible in a timely fashion requires two or more fields per year the first few years after diagnosis, which has proven to be difficult in many clinical settings. This presentation will explain why we recommend that the shorter SITA Faster 24-2 threshold test for those having an HFA3 perimeter, and SITA Fast for those using an old HFA2 perimeter, why SITA SWAP is not recommended at all and 10-2 not recommended as a standard test. The role of SITA Faster 24-2C will also be explained as will the importance of good patient instructions.

What type of ocular anaesthesia should I choose for glaucoma surgery? | Tom Eke
A brief guide to anaesthesia options for your patient’s glaucoma surgery: local anaesthesia with topical/intracameral, sub-conjunctival, sub-Tenon’s, needle block; sedation and general anaesthesia.

What treatments should I offer a patient newly diagnosed with open angle glaucoma? | Chelvin Sng
For newly diagnosed glaucoma, the aim of treatment is to slow or prevent glaucoma progression and to preserve vision-related quality of life during a patient’s lifetime. Lowering of intraocular pressure (IOP) is the only proven and effective treatment and is the mainstay of glaucoma therapy.

What should the ophthalmologists do in the developing world?
Professor Geoff Pollard discussed what the ophthalmologist in the developed world should be doing using Australia as an example He noted that the fastest growing age group was 100 years and more and talked about how this was going to influence glaucoma care. He mentioned that about 2% of the population had glaucoma but only 50% were diagnosed and of these only 50% adhered to their medication therefore only 25% were likely to have been treated. He mentioned that 25% of those who were diagnosed had significant visual impairment or were blind at diagnosis. He described the patients journey from the community before diagnosis to diagnosis and to lifelong management. He concluded that the Ophthalmologists as leaders of the eye team should foster a collaborative approach to care and influence all stages of glaucoma patient care.

What should OCT be telling you about a patients glaucoma
OCT helps evaluate for glaucoma damage and can aid in staging the extent of loss. Still artifacts due to poor signal strength, floaters, parapapillary atrophy to name a few may mimic damage. OCT use in advanced loss is limited due to the floor effect. It is important to understand OCT’s strength and limitations.
From the Education Committee
Dr. Murray Fingeret discussed how to use optical coherence tomography to evaluate glaucoma. Caution should be exercised in the interpretation of RNFL thickness measurements in myopic eyes and in eyes with vitreous floater over the parapapillary region when false positive detection may occur. In eyes with advanced glaucoma, floor effect may limit the detection of progressive RNFL thinning. Understanding the limitations of OCT is important to the management of glaucoma patients.

What is the surgical management of malignant glaucoma? | Part 2 | Ramanjit Sihota
Malignant glaucoma is a recalcitrant glaucoma with very shallow anterior chambers, and often very high IOPs, in the presence of a patent iridotomy. It is variously known as
aqueous misdirection or ciliary block glaucoma, reflecting its pathophysiology.
Shaffer and Hoskins have suggested that aqueous may be misdirected into the vitreous, pushing the lens iris diaphragm forward, and the vitreous face appears to prevent the movement of this aqueous anteriorly. Quigley et al suggest choroidal thickening and supraciliary effusion as the cause for recalcitrant shallowing of the anterior chamber.
The first sign of Aqueous misdirection to look for, is an axial shallowing of the anterior chamber, with a tense eyeball, sometimes even while the surgery is in progress. Aqueous misdirection is accompanied by pain and severe diminution of vision. On examination there is ciliary congestion, an absent or very shallow anterior chamber, corneal stromal and epithelial edema, and a stony hard eye.
If diagnosed early, the IOP may be in the normal range.
The aim of management is to restore aqueous movement across all three chambers of the eye, to permit normal outflow.

What is the surgical management of malignant glaucoma? | Part 1 | Ramanjit Sihota
Malignant glaucoma is a recalcitrant glaucoma with very shallow anterior chambers, and often very high IOPs, in the presence of a patent iridotomy. It is variously known as
aqueous misdirection or ciliary block glaucoma, reflecting its pathophysiology.
Shaffer and Hoskins have suggested that aqueous may be misdirected into the vitreous, pushing the lens iris diaphragm forward, and the vitreous face appears to prevent the movement of this aqueous anteriorly. Quigley et al suggest choroidal thickening and supraciliary effusion as the cause for recalcitrant shallowing of the anterior chamber.
The first sign of Aqueous misdirection to look for, is an axial shallowing of the anterior chamber, with a tense eyeball, sometimes even while the surgery is in progress. Aqueous misdirection is accompanied by pain and severe diminution of vision. On examination there is ciliary congestion, an absent or very shallow anterior chamber, corneal stromal and epithelial edema, and a stony hard eye.
If diagnosed early, the IOP may be in the normal range.
The aim of management is to restore aqueous movement across all three chambers of the eye, to permit normal outflow.

What is the role that Müller glia plays in Glaucoma?

What is the Role of Continuous IOP Monitoring in Daily Practice?

What is the role of astrocytes and microglia in glaucoma?

What is the next step in glaucoma treatment after one medication failed to sufficiently lower IOP? | Makoto Aihara
If 1st line drug FP agonist (PGA) was ineffective, change to another FP agonist. If 1st drug did not reach target IOP, select the 2nd line drugs including combined drugs. Consider the following points to select the next step with drugs.
1. Change to FP/beta combined drugs or add 2nd line drugs including these combined drugs considering the glaucoma stage and target IOP
2. Adverse event and Contraindication for each drug: systemic and ocular
3. Ocular tolerability: decrease the total amount of preservatives
4. Adherence: reduction of the medication burden in point of the number of drops and bottles, comfort, or availability to visit.
5. Select combined drugs if available. Now, 6 kinds of combined drugs classified by MOA are available.
Effective and safe management of glaucoma required the better combination of the prescribed drugs, patient education, environment, and our precise practice.

What is the key to improve adherence in NTG?

What is the impact of Glaucoma on quality of life and how to evaluate this? | Amanda Kiely Bicket
Glaucoma has the potential to negatively impact patients’ quality of life from earliest diagnosis, even before they experience overt visual symptoms.
We serve our patients best by understanding their experiences and priorities, capturing their vision-related quality of life in precise and efficient ways, and continually working to understand and address the impact of glaucoma and glaucoma treatment on their daily lives. There is a substantial body of literature examining quality of life in patients with glaucoma. However, few treatment trials include vision- or health-related quality of life outcomes. Moreover, glaucoma patients tell us that maintaining daily function is their highest priority, but routinely-measured clinical outcomes do not capture patient function well.
This presentation will review available patient-reported quality of life measures and evidence for their use, and will include practical tips for both clinicians and vision researchers aiming to understand quality of life in glaucoma patients.

What is the ideal frequency of Optical Coherence Tomography Testing to Detect Progression in Glaucoma?

What is the current position of MIGS in glaucoma surgery

What is the best way to examine the optic nerve for early detection of glaucoma? | Remo Susanna
The optic nerve examination is the most important component of the evaluation of a glaucoma patient. The appearance of the optic nerve can assist with diagnosing glaucoma and detecting its progression. It is irreplaceable in detecting nonglaucomatous causes of ONH cupping and visual field defects similar to those in glaucoma.
A systematic process of disc examination is presented in this lecture. It enhances the ability to detect glaucomatous damage as well as disease progression.
Computerized imaging techniques such as scanning laser ophthalmoscopy, scanning laser polarimetry, and optical coherence tomography, have been proposed as alternative methods to help the clinician in glaucoma diagnosis. However, they are not able to identify pallor of the neuroretinal rim, disc hemorrhages, or vascular signs of acquired cupping.
These instruments do not provide a better ability to discriminate normal from glaucomatous eyes when compared to glaucoma experts. However, the combination of information provided from subjective and objective analysis can be synergistic.

What is the added value of MIGS to phacoemulsification
Dr. Kerr emphasized on benefits of combining MIGS with cataract surgery. He said the combination achieves lower intraocular pressures with fewer anti glaucoma medications, improves ocular surface disease and quality of life as well. It is also believed to reduce the rate of glaucoma progression and the total cost of treatment.

What is significant progression? Statistically significant versus clinically meaningful

What is glaucoma?
Glaucoma is a chronic, progressive, degenerative disorder of the optic nerve that produces characteristic visual field damage. Glaucoma is the second cause of blindness, and importantly: it is irreversible.
It is estimated that around 80 million people have glaucoma worldwide. Approximately 50% of the individuals with glaucoma are unaware that they have the disease, and this number may be even higher in underdeveloped countries. This is because in its early stages, glaucoma is asymptomatic. If untreated, glaucoma may progress to blindness.
Periodic testing allows early diagnosis to prevent visual disability.
What is AI?
Deep learning algorithms include identification of glaucomatous discs from normal ones by using fundus photographs. Deep learning of the RNFL enface OCT scans has improved the prediction of visual field damage as compared to RNFL thickness. Deep learning of the RNFL enface OCT has also improved the prediction quantitative parameters such as VF MD with high accuracy and lower errors as compared with RNFL.Despite the accuracy, AI comes with certain biases, which can be tackled by development of newer algorithms.

What is a GWAS?
Dr.Ching-Yu Cheng talked about Genome-Wide Association Studies. He mentioned association studies evaluating direct association between risk factors and disease, providing examples of association between family history, genetic factors and glaucoma.

What does OCTA bring glaucoma diagnosis new?

What does Humhrey 24-2C mean to us?

What does Corneal Pachymetry tell me about my patient’s glaucoma risk? | James Brandt
This lecture addresses the known limitations of Goldmann applanation tonometry (GAT), widely regarded as the current reference standard tonometer. Hans Goldmann, the tonometer’s inventor, recognized in the 1950s that if central corneal thickness (CCT) varied widely, GAT would be inaccurate. Only decades later could CCT be measured reliably, and Goldmann’s prediction proved prescient with patients categorized as having ‘normal tension glaucoma’ having thinner CCTs than average, and patients with ocular hypertension having thicker CCTs than average.
Among the primary goals of the landmark Ocular Hypertension Treatment Study (OHTS) was to identify measurable characteristics at baseline that might predict which OHTS participant would go on to develop Primary Open Angle Glaucoma (POAG). GAT was the primary tonometry used in the OHTS. Ultrasonic pachymetry was added to the early measures in the OHTS, in particular after it was recognized that the world’s pachymetry literature was based on patients from Scandinavia and Greenland. With a quarter of the OHTS subjects being of self-described African heritage, an opportunity arose to determine if there were differences in CCT that might underly the increased risk of glaucoma among black patients. In the OHTS, Black subjects as a group had thinner CCTs than their non-Black counterparts.
When the OHTS investigators published the first multivariate predictive model for glaucoma, thinner CCT was its most powerful component – a CCT 40 µm thinner than average predicting a 70% increased risk of developing glaucoma. Thinner CCT increased risk independent of measured IOP or cup-disc ratio.
This model and the subsequent combined OHTS and European Glaucoma Prevention Study (EGPS) risk models perform extremely well in predicting an ocular hypertensive patient’s risk of developing glaucoma. Corneal pachymetry helps the clinician use the OHTS, OHTS-EGPS and other risk models to determine risk in an individual patient.
In large datasets thicker CCT causes an over-estimation bias of Goldmann tonometry whereas thinner CCT induces an under-estimation bias. Although several published ‘correction’ formulas describe this relationship in large datasets, the clinician should avoid being tempted to ‘adjust’ IOP estimates acquired by GAT using CCT measures.
There are 3 reasons clinicians should avoid using so-called ‘correction’ or ‘IOP adjustment’ nomograms in individual patients:
1. Engineering models suggest that the impact of CCT on GAT error is quite modest compared to other factors like corneal hydration, aging, viscoelasticity, and treatment effects; indeed, the influence of these other factors dwarfs CCT, varies based on the true IOP and cannot be modeled with a simple linear equation or correction nomogram
2. CCT can be measured with great precision (± 5 µm, or ± 1% in a 500 µm cornea) whereas in the best of hands the precision of GAT is ± 2.5 mmHg, about ± 10-15% in most patients. Using a precise measurement like CCT to ‘adjust’ a single noisy measurement like GAT makes no sense.
3. Most of the so-called ‘correction’ nomograms are based on linear regressions of cannulation data acquired from healthy eyes undergoing cataract surgery. In the clinic one has no way to know if your patient with a 625 µm cornea has a thick stiff cornea or a thick soft cornea. Without knowing the individual cornea’s material properties, you may adjust GAT-derived IOP in the wrong direction or to the wrong extent.
So how should you use corneal pachymetry to determine your patient’s glaucoma risk? Use the data in one of the published risk models. Just as we’ve learned to think of optic nerves as ‘small’, ‘average’ and ‘large’ when interpreting cup-disc ratio, I recommend you think of CCT in terms of thin (570 µ) when interpreting GAT-derived IOP estimates. Don’t be tempted to ‘adjust’ GAT measurements with CCT.

What do you do? Trabeculectomy tips and tricks of ANZGS surgeons

What do we know about the risk for visual impairment due to primary angle closure?

What do we know about the genetics and IOP?

What did we learn from the EAGLE trial?
For PAC with high pressures, and PACG eyes, phacoemulsification resulted in better quality of life, lower pressures on less medication and was more cost effective than laser iridotomy.
Clear lens extraction should be considered as an option for first-line treatment of PAC and PACG.
From the Education Committee
Dr. Foster quoted studies to show how with increase in rates of cataract extraction and laser iridotomy, the incidence of acute primary angle closure has decreased significantly. He discussed in detail the design and results of EAGLE study. He showed that after 3 years, phaco clear lens extraction resulted in better quality of life, lower pressures on less medication and was more cost effective than laser PI. He concluded by saying that clear-lens extraction should be considered as an option for first-line treatment of PAC & PACG.

What Deforms the Lamina Cribrosa? A Three-Dimensional Investigation
The lamina cribrosa deforms in different magnitude and spatial locations within the 3D volume in response to pressures modulations. Assessment of the anterior surface of the lamina or the response to intraocular pressure modulation is insufficient for full evaluation of the lamina dynamics.

What causes IOP variations

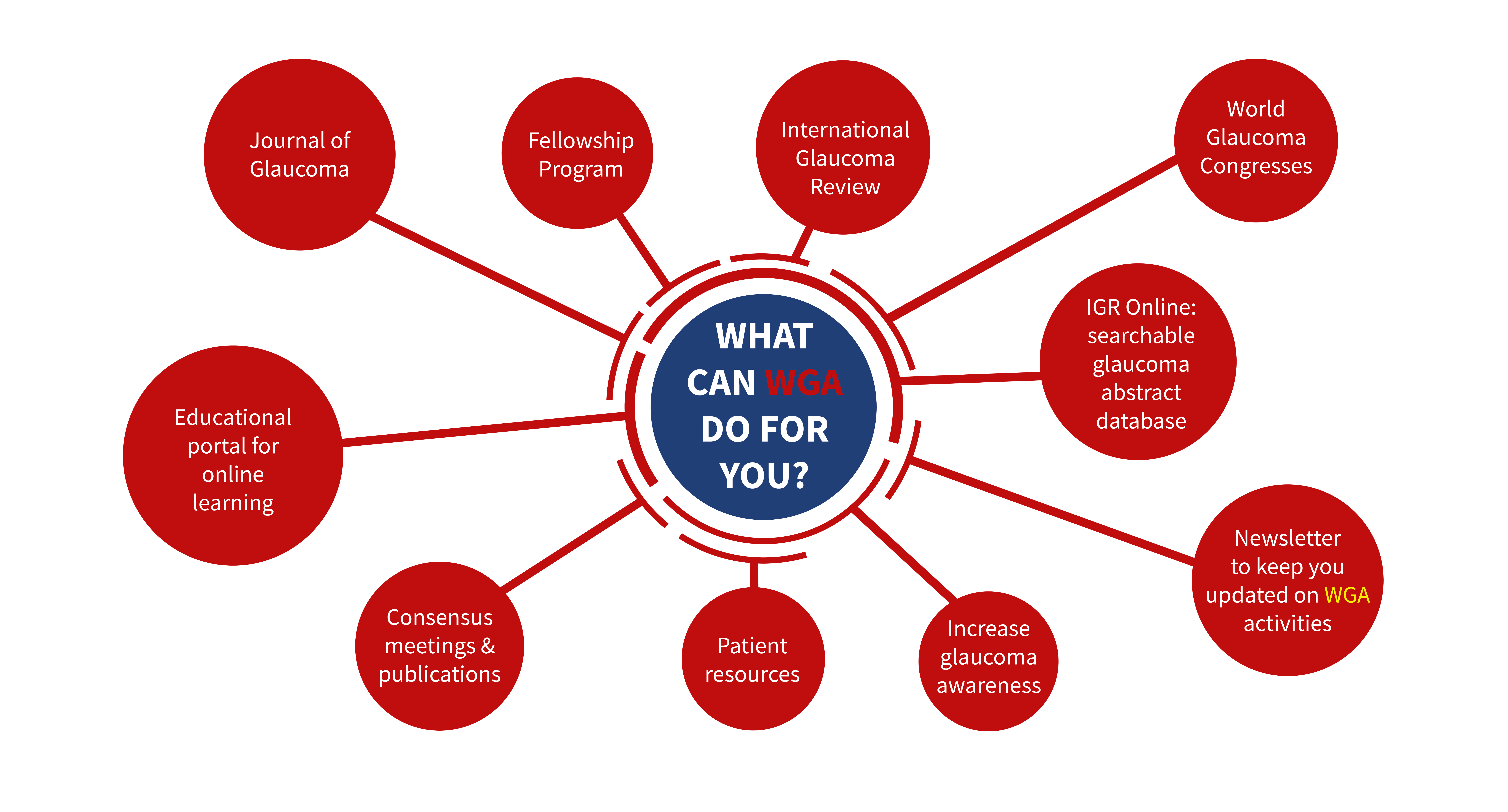
What can WGA do for you?
Membership of the World Glaucoma Association is FREE if you’re a member of one of our affiliated glaucoma societies!
- Belong to a global community: connect with other health care professionals specialized in glaucoma.
- Access top-notch resources: receive free online access to our publications: the International Glaucoma Review (IGR) and the Journal of Glaucoma (JOG) and read the latest news of the WGA in our monthly newsletter.
- Help drive glaucoma awareness: have a voice to advocate for glaucoma and participate in World Glaucoma Week, planned annually in March.
- Experience significant savings: take advantage of a discount on the registration fee for our biennial World Glaucoma Congress (WGC).
- Boost your knowledge on glaucoma: develop your professional standing and that of your institution by using our educational portal, online courses and webinars.
- Experience strength in numbers: gain valuable insights with the Glaucoma Consensus Initiative, based on the idea that the collective wisdom of a group is better than the opinion of a single expert.
- Support your patients: relay unbiased information about glaucoma, using accessible language in a user-friendly platform.
The WGA services
- World Glaucoma Congress
- Increase glaucoma awareness
- Newsletters to keep you updated on our activities
- IGR Online: searchable glaucoma abstract database
- International Glaucoma Review
- Journal of Glaucoma
- Basic Course in Glaucoma
- Educational portal for online learning
- Fellowship Program
- Consensus meetings & publications
- Patient Education Website
What can the ophthalmologists do in the developing world?
Dr. Olawoye discussed the incorporation of counselling units and family screening into glaucoma clinics across Sub Saharan Africa to improve awareness and the use of simple basic instruments for screening and diagnosis of glaucoma at the community, primary and secondary levels. She emphasized the importance of training ophthalmologists to perform good trabeculectomy especially those working in resource constrained settings and advocated for the provision of cheap and affordable low vision aids for those at the end of glaucoma continuum.
From the Education Committee
Olusola Olawoye spoke about the wide continuum of developing countries and focused her discussion on the least developing countries where resources are grossly sparse. She noted from the meta-analysis by Tham et al that Africa and Asia would be responsible for the highest increase in glaucoma prevalence in the future due to an increased life expectancy. She focused mainly on the importance of appropriate, cheap and sustainable approaches to glaucoma care in developing countries.

What can go wrong in MIGS and how to manage

What Artificial Intelligence(AI) means in glaucoma

What are the Main Barriers to Glaucoma Care?

What are the main barriers to glaucoma care in sub-saharan africa
This video emphasized high prevalence and poor awareness of glaucoma in a resource constrained setting as major barriers to glaucoma care. Other barriers are lack of diagnostic equipment, difficulties accessing glaucoma drainage devices and lasers and the impracticality of medical management due to lack of resources. Dr. Olawoye suggested that creation of glaucoma awareness through community eye outreaches and family screening, effective cheaper surgical procedures like trabeculectomy may be ways of overcoming some of these barriers in Sub-Saharan Africa.
From the Education Committee
Dr. Olusola Olwoye discussed the main barriers to glaucoma care in Sub-Saharan Africa, including the prevalence of the disease, scarcity of resources, issues related to diagnosis, management, awareness and finalized her talk with a discussion of what lies ahead?

What are the current recommended treatment options for progressing advanced glaucoma?

What about the Lamina Cribrosa?

What about fast progressing NTG

WGW Newsletter signup
WGC2021 Newsletter signup
WGC-2027 Committee
WGC-2027 – Kyoto, Japan
Save the date for the 12th World Glaucoma Congress (WGC) to be held April, 20-23, 2027, in Kyoto, Japan.
WGC-2025 | Society Symposium Program Submission
Please submit your symposium program information with the below form and keep in mind the below points for your program:
- Your symposium will be 1 hour.
- Ensure to include Q&A and leave enough time for a discussion at the end.
- Your symposium should be held in English.
Deadline to provide the complete information of your symposium is November 8, 2024
Should you have any questions, please do not hesitate to contact the WGC-2025 Team at wgc@mci-group.com.
WGC-2025 | Society Representative at President’s Dinner
WGC-2025 | Poster Certificate
WGC-2025 | General Assembly Registration
Registration for WGA General Assembly is closed.
We are looking forward to welcoming you in Honolulu, Hawaii.
WGC-2025 | Consensus Meeting attendance
Registration for WGA Consensus Meeting is closed.
We are looking forward to welcoming you in Honolulu, Hawaii.
WGC-2025 | CME Survey
WGC-2025 | CME Authorization
To access the survey and certificate, please enter below your registration identifier (which can be found on your badge or confirmation email) and the email address used during your registration.
Should you have any further questions, please do not hesitate to contact us via email.
WGC-2025 Program Faculty Invitation
Kindly log-in to your WGA#One Account to continue with the RSVP.
Note: If you don’t have a WGA#One account or you have forgotten your password, simply click the “Log In” button below, then select “Create an account” or “Forget Password” at the bottom.
Email us at wgc@mci-group.com should you have any questions.
WGC-2025 – Honolulu, Hawaii, USA
From June 25–28, over 1,800 glaucoma specialists and eye care professionals from across the globe gathered in Honolulu, Hawaii for the 11th World Glaucoma Congress (WGC) – our most ambitious and inclusive congress to date.
Over four unforgettable days, we brought together clinicians, researchers, and industry leaders from around the world. From hands‑on wet labs to packed panel discussions, every moment reflected the strength and diversity of our global glaucoma community.
We are deeply grateful to our Program Planning Committee (PPC), and extend our sincere thanks to the PPC Co-Chairs, Dr Pradeep Ramulu and Dr Tanuj Dada, for arranging a superbly curated scientific program.
Downloads
Photo Galleries
- Tuesday, June 24, 2025 – Consensus Meeting
- Wednesday, June 25, 2025
- Thursday, June 26, 2025
- Friday, June 27, 2025
WGC-2023, Rome, Italy
Aftermovie
Downloads
Photo Galleries
The 10th World Glaucoma Congress (WGC) was held at the La Nuvola Convention Center from June 28 – July 1, 2023 in Rome, Italy. The 10th World Glaucoma Congress was the largest glaucoma meeting held anywhere in the world to date, as we welcomed over 3100 ophthalmologists and allied health professionals from more than 100 different countries.
The scientific program was composed of an inspiring variety of symposiums, courses, workshops, wetlabs, rapid fire sessions and poster walks covering topics from the basic science and genetics of glaucoma, to the latest developments in medical and surgical management of glaucoma. A technical exhibit area was available to learn about the latest diagnostic and therapeutic technologies and possibilities.
WGC-2023 | New CME Certificate
WGC-2023 | General Assembly
On behalf of Neeru Gupta, WGA President, we are pleased to invite you to the General Assembly of Glaucoma Societies during the 10th World Glaucoma Congress, in Rome, Italy.
General Assembly
Date: Wednesday, June 28, 2023
Time: 14:30 – 15:30 CEST
Venue: La Nuvola Convention Center, Rome, Italy
Location: Room C
WGC-2023 | CME Survey
WGC-2023 | CME Registration
WGC-2023 | CME Authorization
To access the survey and certificate, please enter below your registration identifier (which can be found on your badge or confirmation email) and the email address used during your registration.
Should you have any further questions, please do not hesitate to contact us via email.
WGC-2023 Committee
WGC-2023 Call for Topics
WGC-2021: Going Deeper
The WGA Global Webinar series returned on Saturday, October 9, diving into trailblazing glaucoma research presented at the WGC-2021.
The 6th webinar featured the very best of WGC-2021, with new discussions going deeper into these topics:
- Is Normal Tension Glaucoma a separate entity from Primary Open Angle Glaucoma?
- NTG: blame it on your parents (and their genes)
- Myopic optic neuropathy or GON?
- Clinical relevance of 24 hs IOP monitoring
- How glaucoma affects patients
- Early lens extraction in PAC/PACG after/without LPI

WGC-2021, E-Congress
Downloads
The 9th World Glaucoma Congress was held virtually hosted by the Japan Glaucoma Society (JGS) from June 30 – July 3, 2021. We virtually conducted 70+ sessions with 40 hours of live broadcast. We welcomed over 350 speakers from 63 countries.
Beyond Borders offered educational exchanges, scientific news, and best practice updates. The congress covered topics from basic science and genetics of glaucoma to the latest developments in the medical and surgical management of glaucoma.
WGC-2021 Patient Symposium
Chair(s): Takeo Fukuchi (Japan); David Friedman (United States)
- 00:00 – 00:05 – Introduction (Takeo Fukuchi, Japan)
- 00:05 – 00:13 – How we are able to help patients with glaucoma: Glaucoma Australia (Annie Gibbins, Australia)
- 00:13 – 00:21 – Engaging patients during WGW and other ways to help your patients (Ana Maria Vasquez Garcia, Ecuador)
- 00:21 – 00:29 – How glaucoma has changed my life (Nobuko Nakamura, Japan)
- 00:29 – 00:38 – For more mutual understanding between glaucomatous patients and ophthalmologist (Tetsuya Yamamoto, Japan)
- 00:38 – 00:46 – Invited lecture (Daiko Matsuyama, Japan)
- 00:46 – 01:00 – Discussion and Q&A (David Friedman, United States)

WGC-2021 Committee
WGC-2021 Beyond Borders
9th World Glaucoma E-Congress
WGC-2021 Beyond Borders will offer educational exchanges, scientific news, and best practice updates. The congress will cover topics from basic science and genetics of glaucoma, to the latest developments in the medical and surgical management of glaucoma. It will be virtually hosted by the Japan Glaucoma Society (JGS).
Register now and save.

WGC-2021
This is the original message presented at WGC 2019 Melbourne for WGC-2021 Kyoto joint-meeting with Japan Glaucoma Society annual meeting. Please mark the calendar and attend the meeting with us!

WGC-2019, Melbourne, Australia
Downloads
Photo Galleries
The 8th World Glaucoma Congress was held at the Melbourne Convention and Exhibition Centre (MCEC) from March 27–30, 2019 in Melbourne, Australia. We welcomed over 2000 ophthalmologists and allied health professionals from more than 90 different countries.
The scientific program was a stimulating mix of symposiums, courses, workshops, wetlabs, rapid fire sessions and poster walks covering topics from the basic science and genetics of glaucoma, to the latest developments in medical and surgical management of glaucoma
WGC-2019 Film Festival
The Film Festival aims to put storytelling power in the hands of glaucoma experts and seeks to showcase the role of individuals and communities as champions for glaucoma prevention, diagnosis and treatment. The festival offers a versatile way to learn and spark the conversation about glaucoma in creative ways. It features films directly or indirectly related to glaucoma, that explore and highlight the disease locally, nationally and globally. Our goal is to screen films that demonstrate, educate, inspire and encourage a change, to eliminate blindness and visual disability due to glaucoma around the world.
The top 30 film submissions as judged by the Program Planning Committee were shown in the Film Theater at least twice during the World Glaucoma Congress in Melbourne and special prizes were awarded to the three winning films. You can now view them online from the comfort of your own home, on any device. Keep an eye on the WGC-2021 website to see when submission for the next Film Festival opens.
- First Prize: “Bleb Rescue Operations” by Talvir Sidhu, India
- Second Prize: “iStent Inject – How to deal with overimplantation” by Bryan Ang, Singapore
- Third Prize: “How to fix and prevent a short tube” by Daniela Alvarez-Ascencio, Mexico
Disclaimer
The Hippocrates Glaucoma Foundation, based upon an agreement with the World Glaucoma Association, organizes the World Glaucoma Congress with the aim of providing education and scientific discourse in the field of glaucoma. The Hippocrates Glaucoma Foundation and World Glaucoma Association accept no responsibility for any products, presentations, opinions, statements, or positions expressed by speakers at the congress. The inclusion of material in the scientific program does not constitute any endorsement by The Hippocrates Glaucoma Foundation and World Glaucoma Association. Material includes, but is not limited to, abstracts (PowerPoint/Keynote), presentations, videos, audio files, (Film Festival) films, and hard copy handouts.
WGC-2019 Committee
WGC-2017- Film Festival
Videos presented at the film festival during the World Glaucoma Congress in Helsinki, Finland from July 17 – 20, 2017.
WGC-2017 Presentations: Education Committee Selections
The Education Committee carefully selects presentations which are made accessible to everyone!
We are continuing with a WGC-2017 summary of Eytan Blumenthal. Five interesting talks discussing how to challenge glaucoma in very low-income populations
Session 1: Advanced glaucoma in low-income populations
Five interesting talks discussing how to challenge glaucoma in very low-income populations.
First, Dr. Philippin discussed various approaches on how to raise public awareness in general and patient awareness in particular.
Dr. Catherine Green discussed how to train eye care providers, highlighting the fact that money alone will not solve the problem, and that attention should be addressed to how and not only to what must be learned, and concluded with a description of the “Pacific Islands project”.
Dr. Sheila Marco from Kenya next highlighted the role of technology, concentrating on equipment needed for diagnosis, distinguishing what might be considered a must and what is merely “nice to have” in their setting.
Dr. Tony Realini discussed what sustainable effective treatment options are, highlighting the limitations of each option in the low-income population setting. One promising option discussed is the SLT with its safety profile. Efficacy data from a low-income environment is presented.
Last, Dr. G Chandra Sekhar concluded the session discussing cost effective glaucoma programs. One such screening & treatment program is described in detail, based on a structured system of referrals from Vision Guardians to Vision Centers to Secondary Eye Care Centers, utilizing telemedicine and even “Drone slit-lamps”.
Session 2: Africa Symposium
Five fascinating lectures discussed the unique constraints and opportunities of managing glaucoma in the African continent.
First, Dr. Neeru Gupta discussed the magnitude of the problem in sub-Saharan Africa and introduced Dr. Eddie Kgao Legodi who overviewed initiations as well as the WOC scheduled for 2020 in South Africa.
Dr. Olusola Olwoye discussed the main barriers to glaucoma care in Sub-Saharan Africa, including the prevalence of the disease, scarcity of resources, issues related to diagnosis, management, awareness and finalized her talk with a discussion of what lies ahead?
Next; Dr. Keith Martin characterized the major management challenges, including: late presentation, adherence to treatment, the level of training of trained personnel, identifying avoidable/preventable blindness, and ways of bringing in support and knowledge.
Dr. Dan Kiage discussed the surgical approach and the unique considerations in Africa separately for each of the glaucoma surgical procedures.
Last, Dr. Fatima Kyri discussed lessons learned from the treatment of glaucoma in Nigeria, and described a framework for treating glaucoma in this country, as well as implications for better controlling glaucoma.
Dr. David Friedman concluded the session.
Session 5: Biomechanics in glaucoma
Dr. Cynthia Roberts opened the session with an in depth discussion of corneal biomechanics as it pertains to measuring IOP and understanding measurement artefacts. Newer tonometers are discussed in the context of corneal biomechanics.
Dr. Michael Girard described the biomechanics of the optic nerve as it pertains to glaucoma pathogenesis. Biomechanics of the optic nerve head and deformations were modeled using OCT, MRI & animal data incorporated into a finite-element model. Implications related to the concept of “stiff” dura, sclera and optic nerve are described.
Dr. Darryl Overby next discussed the biomechanics of the trabecular meshwork, presenting a hypothesis of outflow homeostasis involving an active mechanism regulating trabecular meshwork resistance, involving concepts such as trabecular meshwork stiffnes, shearing forces, nitrous oxide and feedback mechanisms.
Last, Dr. Paul Kaufman discussed in depth the biomechanics of presbyopia as it pertains to glaucoma. Beyond a loss of lens elasticity with age, a restrictive aging of the muscle is shown to be secondary to scarring within the ciliary muscle, all leading to presbyopia. A case is made that the ciliary muscle and choroid form an elastic network that extends from the TM to the optic nerve region, mobilized by accommodation, and relevant to the pathogenesis of glaucoma.
WGC-2017 Helsinki, Finland
Downloads
Photo Galleries
The 7th World Glaucoma Congress was held at the Messukeskus Helsinki, Expo and Convention Centre from June 28–July 1, 2017 in Helsinki, Finland.
The 7th World Glaucoma Congress was the second largest glaucoma meeting held anywhere in the world to date. Following the successful Congresses in Vienna, Singapore, Boston, Paris, Vancouver and Hong Kong, WGC–2017 was open to all glaucoma care providers including glaucoma specialists, visual scientists, clinicians, other ophthalmologists, optometrists, nurses, technicians, and others with an interest in glaucoma.
WGC-2017 Committee
WGC-2015 Hong Kong
Downloads
Photo Galleries
The 6th World Glaucoma Congress was held at the Hong Kong Convention and Exhibition Centre from June 6-9, 2015 in Hong Kong, China.
Following the successful Congresses in Vienna, Singapore, Boston, Paris and Vancouver, WGC–2015 was open to all glaucoma care providers including glaucoma specialists, visual scientists, clinicians, other ophthalmologists, optometrists, nurses, technicians, and others with an interest in glaucoma. A technical exhibit area was available to learn about the latest diagnostic and therapeutic technologies and possibilities.
WGC-2015 – Film Festival
Videos presented at the film festival during the World Glaucoma Congress in Hong Kong from June 6 – 9, 2015.
WGC-2013 Vancouver
Downloads
Photo Galleries
The 5th World Glaucoma Congress was held at the Convention Centre in Vancouver, Canada from July 17 – 20, 2013. The World Glaucoma Association was pleased to host this World Congress together with the local host, the Canadian Glaucoma Society.
Following the successful Congresses in Vienna, Singapore, Boston and Paris, WGC-2013 was open to all glaucoma care providers including glaucoma specialists, other ophthalmologists, optometrists, nurses, technicians, and others with an interest in glaucoma. A technical exhibit area was available to learn about the latest diagnostic and therapeutic technologies and possibilities.
WGC-2013 – Film Festival
Videos presented at the film festival during the World Glaucoma Congress in Vancouver, Canada from July 17 – 20, 2013.
WGC-2011 Paris
Downloads
Photo Galleries
The 4th World Glaucoma Congress was held at the Palais des Congrès in Paris, France from June 29 – July 2, 2011. The 4th World Glaucoma Congress was the third largest glaucoma meeting held anywhere in the world to date.
On behalf of the World Glaucoma Association, its Board of Governors and the World Glaucoma Congress Organizing and Program Committees, it was with great pleasure that I invited you to participate in the World Glaucoma Congress in Paris on June 29-July 2, 2011. The Organizing and Program Committees have worked along with clinicians, researchers and leaders in our field to create an innovative, interactive meeting in a wonderful setting.
More than 70 glaucoma societies from throughout the world were represented, and shared their experiences, knowledge and creativity. Didactic sessions, basic and clinical science sessions, symposia and debates, courses, and posters have all created a most memorable meeting.
WGC-2009 Boston
Downloads
WGC-2005 Vienna
Downloads
WGC | Registration Status
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login
WGC PPC Co-Chair Nominations Form
The deadline has now passed and nominations are no longer being accepted. Thank you.
WGC meta data entry form
WGC 2021 Speaker Info Script
WGC 2019
World Glaucoma Congress 2019
A globally diverse faculty of experts in glaucoma research and clinical practice will come together to share their knowledge and insight in Melbourne, Australia, from March 27-30, 2019. We welcome you to be a part of the principal congress focused on the education of glaucoma. Scientific sessions will include 21 symposiums, 24 courses, grand rounds, film festival, rapid fire presentations, and the largest surgical wetlabs in the field of glaucoma.


WGC 2015 Hong Kong
The 6th World Glaucoma Congress will be held at the Hong Kong Convention and Exhibition Centre from June 6 – 9, 2015.
The World Glaucoma Congress is the largest glaucoma meeting held anywhere in the world to date. Following the successful Congresses in Vienna, Singapore, Boston, Paris and Vancouver, WGC–2015 will be open to all glaucoma care providers including glaucoma specialists, visual scientists, clinicians, other ophthalmologists, optometrists, nurses, technicians, and others with an interest in glaucoma. A technical exhibit area will be available to learn about the latest diagnostic and therapeutic technologies and possibilities.
Hong Kong is a city that connects East and West in a décor of history, business and tremendous natural beauty. The Organizing Committee invites you to join us in Hong Kong from June 6 – 9, 2015 for World Glaucoma Congress 2015!
- January 18, 2015: Abstract submission deadline
- March 31, 2015: Early registration
- June 6 – 9, 2015: Congress dates
WGA#One Management System
WGA#One contains detailed information about all affiliated Glaucoma Societies and Glaucoma Industry Members.
Primary contacts of both types of organizations are able to modify and update their own organization details at any time by using their login details.
Via this system you are able to:
- Check and if necessary adapt your organization profile, published via the WGA website (will be live end of June)
- View members/representatives of your organization*
Affiliated Societies only:
- Add annual meetings to the on-line Meeting calendar available via WGA website
- Check, add or if necessary adapt your Board members details published via the WGA site as well*
*For adjustments, please contact the WGA Executive Office (info@worldglaucoma.org
How to log in
If you are the primary contact for your society, you will see the option to switch to your society profile after you are logged in to your own profile.
Contact the WGA Executive Office (info@worldglaucoma.org should you require assitance, or wouldlike to add members to your society.
WGA#One and WGA Journals
WGA’s online platform provides easy and free access to a host of educational material in glaucoma.

WGA | Surgical Grand Rounds | November 30, 2023
Program November 30, 2023
- Choroidal Detachment presented by Sameh Mosaed, MD (United States). Panelists: Liza Sharmini, MD (Malaysia) and Catherine Jiu-Ling Liu, MD (Taiwan). Moderated by Pradeep Ramulu, MD (United States).
- Suprachoroidal Hemorrhage after Glaucoma Surgery presented by Saurabh Verma, MD (India). Panelists: Christina Weng, MD (United States) and Paul Healey, MD (Australia). Moderated by Tanuj Dada, MD (India).
Q&A

Dr. Weng, how long can we wait with kissing choroidals before surgical intervention? 2-3 weeks?
Thanks for your question. I’m assuming you’re asking about a serous choroidal detachment…with kissing choroidals, it’s usually to surgically intervene promptly (usually a matter of days), as those appositional areas can become adherent. For hemorrhagic kissing choroidals, a bit tricky—you want to take them promptly, but need to wait for the heme to be liquefied, so I generally still try to wait a week or so and follow those patients with B-scan ultrasound to identify the earliest point I can intervene. Hope that helps.

Dr. Mosaed, what tecnic is used when you re-ligature a tube?
The tube can be re-ligated using 8-0 suture by making a small incision in the conjunctiva posterior to any patch graft material. If choosing a nylon suture, this can be cut using argon laser at six weeks after the ligature is placed to allow capsule formation around the plate. Alternatively, an 8-0 polyglactin suture can be used which will dissolve at around 6 weeks. The suture should be tied quite tightly to complete ligate the tube, blocking any filtration during this period of capsule formation.

Dr. Verma, if we suture the sclerostomy port how will further drainage occur?
Eye has the capacity to clear blood from suprachoroidal space. Most common indication of drainage is appositional hemorrhagic choroidal detachment. Purpose of drainage is to resolve appositional state of choroidal mounds and reduce the chance of complications such as retinal detachment due to retino-retinal adhesions and high IOP induced optic nerve damage. Once the appositional state is resolved, remaining blood in suprachoroidal space is slowly absorbed. This occurs by liquefaction of blood, hemolysis and transportation of debris by macrophages. Hence, continuous drainage of blood from a sclerostomy site is not required even when complete resolution of suprachoroidal blood is not achieved by drainage.

WGA | Surgical Grand Rounds | January 26, 2023

WGA videos
WGA video
WGA Symposium on Glaucoma and non-IOP related risk factors
The WGA is organizing a symposium on glaucoma and non-IOP related risk factors during the 15th congress of the European Glaucoma Society, on Sunday, June 5, 2022, from 15:45 to 16:45 in the Socrates room.
The program can be found below.
Hosted by: Shan Lin (USA), WGA Executive Vice President
Chaired by: Ingrida Janulevičienė (Lithuania) and Zeynep Ozturker (Turkey)
- Blood pressure and progression of glaucoma | Luciano Quaranta (Italy)
- Using artificial intelligence to detect non-IOP related risk factors in glaucoma | Alon Harris (USA)
- Oxidative stress and inflammation in glaucoma | Miriam Kolko (Denmark)
- Neurorecovery in glaucoma – myths and reality | Tanuj Dada (India)
Please note that in order to be able to attend this symposium, you must be registered for the 15th EGS congress.
For more information and registration visit: https://egs2022.org/registration/
WGA Symposium during WOC 2022
Hot Topics in Glaucoma
The World Glaucoma Association is hosting a session during the 2022 World Ophthalmology Congress on Friday, 9 September at 19:45-20:45 (Central European Summer Time). Check your local time here.
The session “Hot Topics in Glaucoma” will be hosted by Tanuj Dada (India), Shan Lin (United States) and Anja Tuulonen (Finland) and will include the following presentations:
For more information & registration, please visit: https://icowoc.org/congress-information/
WGA Surgical Grand Rounds | September 19, 2024
6th edition of Surgical Grand Rounds – September 19, 2024
Thank you for joining the 6th Surgical Grand Rounds. Recording of the webinar will be available to all in November.
- Avoiding/managing the infected bleb post Trabeculectomy presented by Vivek Dave, MD (India). Panelists: Winnifred Nolan, MD (United Kingdom) and Kuldev Singh, MD (United States). Moderated by Tanuj Dada, MD (India).
- Avoiding/managing infections after subconjunctival implants (XEN/Preserflo/Long tubes) presented by Davinder Grover, MD (United States). Panelists: Kaweh Mansouri, MD (Switzerland) and Jennifer Fan Gaskin, MD (Australia). Moderated by Pradeep Ramulu, MD (United States).
Q&A

Dr. Grover, very nice presentation. Do you symblepharon while with fornical pedical?
No. This is very different from a Symblepharon. One can actually pass a spatula between the proximal portion of the pedical flap and the conjunctiva. The distal end of the flap is healed over the tube. The pedical flap does not create any tension or issues with mobility either.
Please see:
Grover DS, Merritt J, Godfrey DG, Fellman RL. Forniceal conjunctival pedicle flap for the treatment of complex glaucoma drainage device tube erosion. JAMA Ophthalmol. 2013 May;131(5):662-6. doi: 10.1001/jamaophthalmol.2013.2315. PMID: 23699841.” FOR A FULL DESCRIPTION OF THE TECHNIQUE AND THE OUTCOMES ETC.
Dr. Grover, can you detach the conjunctival flap from its base after a couple of months?
One can detach the conjunctival flap from its base after a few months, but we have not done this nor do we advocate for this. Usually, these cases required recruitment of a new blood vessel into an area that has compromised blood flow. Our concern with amputating the base would be that one may cause loss of blood supply and compromise the integrity of the flap.
Dr. Grover, for tube exposure, I have been using free conjunctival graft to cover the corneal tissue which is easier than a pedunculated flap with postoperative systemic oxygen therapy to enhance vascular growth?
We feel, as based on our discussion in the paper above, that a free conjunctival flap is not the best way to take care of this issue. Completely amputating the blood supply will likely lead to a repeat erosion of the tube, as evidenced by studies that report outcomes on this technique. These areas of erosion usually have vascular compromise and one unique aspect of this technique is the recruitment of robust and healthy vasculature into an area deprived of adequate perfusion. A free flap does the opposite and more likely to fail, based on our experience and the published literature.

Thanks a lot Dr. Fan Gaskin! How long after XEN implantation do you prescribe steroids?
I tailor the topical corticosteroid use based on the inflammatory response (vascularity) of the bleb and underlying risk factors for fibrosis of each individual patient but it would usually range between 1-3 months postoperatively at a tapering dose, depending on each case.

WGA Surgical Grand Rounds | July 7, 2022
Program July 7, 2022
- Malignant Glaucoma presented by Leon Au, MD (United Kingdom). Panelists: Harry Quigley, MD (United States) and Esther Hoffmann, MD (Germany). Moderated by Tanuj Dada, MD (India).
- Nanophthalmos with Glaucoma presented by Shamira Perera, MD (Singapore). Panelists: Sharmila Baburajendran, MD (India) and Mohammed Pakravan, MD (United States). Moderated by Pradeep Ramulu, MD (United States).
Q&A

Dr Dada, any role for Chandler’s procedure?
Chandler used a needle to perform fluid vitreous aspiration, however this technique is not currently recommended as an IZHV or a pars plana vitrectomy is performed with a vitrectomy probe.

Dr Au, would a malignant glaucoma present with choroidal detachments?
Generally not, unless it’s choroidal effusion syndrome with subsequent AC shallowing. According to Harry the mechanism seems very similar and certainly similar sort of eyes and risk factors.
Dr Au, what drugs can induce the mechanism of malignant glaucoma?
I’ve only come across topiramate which can cause secondary angle closure, with choroidal expansion and culinary body rotation. Prob similar mechanism as malignant glaucoma.

Dr Hoffmann, would a B scan show fluid pockets of malignant glaucoma?
Yes, sometimes this is visible.

Dr Quigley, is sudden shallowing of anterior chamber during surgery a cause for malignant glaucoma or is the shallow anterior chamber a consequence of suggested mechanisms of malignant glaucoma?
The flattening of the chamber is a consequence of choroidal expansion and poor vitreous flow conductivity as explained.

Dr Perera, would a primary IZH help in nanophthalmic cataract surgeries?
I personally would try not to open the vitreous cavity. I would stick to a more traditional approach like mentioned in the video.
Dr Perera, what IOL formula to you use to decide on the IOL power?
Barret universal II or SRK-T if you are planning for a single IOL placed in the bag. Inherently in these eyes there are some unpredictable results and this must be discussed with the patient.

Dr Rajendrababu, when do you do a limited vitrectomy before cataract surgery in nanophthalmos with angle closure glaucoma as opposed to a sclerostomy?
Role of vitrectomy in nanophthalmic eyes is still not clear. I always prefer a scletostomy over a vitrectomy in these eyes. However there are certain situations when I chose a vitrectomy like the eye is extremely short and AC is flat where surgery via anterior route is risky. In situations where there is sudden rise in intraoperative vitreous pressure not allowing to proceed with surgery through limbus, a limited vitrectomy helps. Performing a needle guided vitreous tap is also not advisable. As the cataract might not allow the visualisation and doing a blind vitrectomy may cause hypotony, retinal tears, vitreous incarcerations, etc.
Dr Rajendrababu, does a sclerostomy have to be so posterior (by the vortex veins)? Or is a more anterior sclerostomy enough?
A posterior scletostomy is done posterior to the insertion of recti muscle and the sclera on this region is slightly thinner than the anterior to equator. It is also easier to penetrate the suprachoroidal space here as there is decompression of sclera and increased permeablility exposing the choroid below & allow continuous egress of uveal effusions. The most dependant portion of the eye is close to the vortex veins and hence a posterior scletostomy will allow the fluid to drain better in this region. Excision of the large sclera beds at the site of vortex veins was sufficient to help resolve excisions without actually performing a vortex decompression as opposed to an anterior sclerostomy.

Dr Pakravan, is it possible to see lens dislocation after IZH?
Yes, potentially, it may rarely happen, however, the damage of zonu;es is minimal and I have seen only a case of Pciol dislocation in a case of severe pseudo exfoliation. Just I reiterate and emphacize that this technique can be used only in pseudophakic eyes.

WGA Surgical Grand Rounds | January 27, 2022
Program January 27, 2022
- Treatment of bleb dysesthesia/overhanging blebs presented by Paul Palmberg. Panelists: Yvonne Buys and Peng Khaw. Moderated by Tanuj Dada.
- Pseudoexfoliation glaucoma with small pupil and cataract with zonular weakness presented by Arsham Sheybani. Panelists: Antonio Fea and Marlene Moster. Moderated by Pradeep Ramulu.
Q&A

Dr. Palmberg, what are the chances of bleb leak when we just snip a bleb overhanging the cornea with Vannas scissors at the slit lamp?
My experience was that only one of the first 13 cases leaked. From that leak case I realized that one needed to carefully examine the portion to be excised using a thin slit beam angled to the side to look for structure within the bleb. If the contents of the bleb was entirely hydrated Tenon’s capsule tissue, it is safe to excize without need for a horizontal compression suture. IF, on the other hand, the portion of the bleb to be removed is optically empty, thus just aqueous filled, a compression suture is placed before excision to prevent leak.
Dr. Palmberg, when doing compression sutures for a dysesthetic bleb, why don’t you use absorbable sutures since having to remove the nylon sutures a second time exposes the patient to a risk of infection?
None of the hundred or so patients in whom I placed nylon compression sutures for a painful bleb and covered them with Polytrim 4 times a day became infected. (One patient in whom I placed a stitch to wall off a lateral leak in a bleb and he did not use the prescribed Polytrim did get a bleb infection and endophalmitis.) The stitch is removed by cutting it with a 30g needle on one side of the corneal portion and grasped at the other end of the corneal portion with Jeweler’s forceps and pulled out straight along the corneal surface (not lifting up). In that way bleb leaks were avoided.
I used nylon since it does not stimulate inflammation, as does vicryl, and the goal is to stimulate the formation of collagen cords in the bleb, not to cause inflammation, which could affect bleb function. Also, braided vicryl would likely abraid the conjunctiva, which could cause a leak. Also, one want the suture to last up to 3 weeks, and vicryl on the surface might be digested before the desired effect occurs. However, in one case, when a patient told me he could not return for follow up as he needed to return to Haiti immediately, I did use a monofilament 8-0 vicryl compression suture, but I have no follow up.

Dr. Khaw, when performing trabeculectomy, does the site (Superior / Superionasal) and number of clock hours of conj-tenon’s dissection influence the occurrence of dysesthesia?
If the superonasal is too near the lid margin then the bleb will more likely be interpalpebral with dysaesthesia. Minimise the anterior clock hour dissection and maximise the posterior pocket to achieve diffuse non-dysaesthetic blebs.
Dr. Khaw, what do think is the main contributing factor to bleb dysesthesia?
Dysaesthesia is mainly caused by the bleb position (interpalpebral and anterior= worse) and the shape of the bleb (high with cystic components). This has effects on the tear film, conjunctival and cornea nerves and sensation causing dysaesthesia. A posterior diffuse bleb under the lid is generally a very comfortable bleb.

Dr. Buys, is your approach to bleb dysesthesia the same if the eye is also hypotonous?
The combination of bleb dysethesia and hypotony typically will require an intervention and on a more urgent basis specifically if vision is affected and/or there is evidence of hypotonous maculopathy. First look for a bleb leak or sweating. In this case address the bleb. Typically they are avascular blebs so suturing or gluing the leak is unlikely to work. One could also consider an autologous blood injection. The definitive approach is to replace the conjunctive either with a pulldown or a conjunctival transplant. If the conjunctive is intact, then the problem is aqueous getting out of the eye from the scleral flap. My suggestion in this scenario is transconjunctival resuturing of the scleral flap. This requires that you can see the sclera. Typically several sutures are required.

Dr. Sheybani, in the case you presented, where a small capsulorhexis had been completed by the outside doctor, but the case aborted because of severe zonular instability, why did you not enlarge the small continuous capsulorhexis?
There was already phimosis forming. Cornea was too cloudy to rush in to surgery so this was 3 weeks after phaco. Concern is that if there is phimosis, it might not tear without running out.
Dr. Sheybani, what nuclear disassembly technique do you favor in an eye with zonular weakness from PXF?
Whichever technique you’re most comfortable with. I prefer horizontal chop for most lenses. A combination of sculpt and chop if the lens is very very dense. I usually do a hemi flip technique.
Dr. Sheybani, what about doing an ICCE and putting an AC IOL (angle or iris supported) in a patient with significant subluxation?
Definitely an option! Keeping the bag is more critical of your wanting to do a mfiol or toric.

Dr. Moster, how do you cortical clean-up in PXF eyes without creating further problems? Any specific technique to remove PXF material?
I do cortical cleanup with a silicon (white tip on the alcon i/a) and pull the cortex east to west or west to east without removing it radially toward the middle like i usually do. I also go close to the angle when removing the visco, and if the bag is stable use a silicon squeegee tip to clean under the anterior capsule ring so as to remove as much psxf as possible. I like to leave the capsule and the angle without any debris.
Dr. Moster, do you ever consider an IOP-lowering procedure in PXF, even if the pressure is not yet high?
Good question. I must say I don’t see many of those as I am a tertiary referral. However, if the iop is normal, the vf, oct, pacy, historesis, family hx, is all normal, I think a perfect phaco, with excellent bag clean up, especially under the anterior capsule ring, and good removal of the visco from the angle is all you will need. Basically, if it isn’t broken, don’t fix it!

Dr. Fea, what is the ideal time to put in a capsular tension ring?
The general suggestion is to implant as late as possible, because the CTR can make the aspiration of cortex more complex, but the final decision is mainly a matter of “feeling” and experience. Especially in subluxated cataracts the posterior capsule can move much more towards the aspiration tip, so in case you feel not at ease, it is definitely better to work a little more and have an intact capsule than to have a subluxated lens with a broken capsule.

WGA Surgical Grand Rounds | Broadcast
WGA 7th Surgical Grand Rounds | Jan 29, 2026
The webinar broadcast has now wrapped up. Thank you all for joining us. We hope you enjoyed the session.
Our experts will review and address all the questions submitted during the broadcast. Their answers will be published on the WGA website in the coming weeks.
The on‑demand replay is available below in case you missed the live webinar or would like to watch it again.
Industry Support
We would like to recognise the ancillary support of our Industry partners in bringing the 7th edition of WGA’s Surgical Grand Rounds webinar to life.
WGA Surgical Grand Rounds | April 14, 2022
Program April 14, 2022
- Managing hypotony after trabeculectomy, presented by Vijaya Lingam. Panelists: Vital Costa and Paul Healey. Moderated by Tanuj Dada.
- Managing hypotony after tubes, presented by Keith Barton. Panelists: Steve Gedde and Anne Coleman. Moderated by Pradeep Ramulu.
Q&A

Dr. Lingam, can you mobilize sclera from adjacent site to close the gap?
Yes, definitely it is an option. Mobilizing the partial thickness scleral flap adjacent to the trabeculectomy scleral flap can be considered if the trabeculectomy flap is dehiscent. In cases where trabeculectomy scleral flap is intact it is not required. Recommended site will be lateral to trab site, use one or two 10 O nylon sutures to anchor the newly created partial thickness after covering the trab site. This will allow aqueous flow and will prevent failure of the bleb. Once it is done there will be need for either conjunctival patch graft or advancement of conjunctiva.
In which situation would you like to inject blood versus compression sutures or bleb repair.
In general compression sutures work best for over filtering blebs. Autologus blood works mainly for localized single leaks, if there is an exuberant bleb with possible localized leak they both can be combined. Bleb repair is recommended for the blebs with extensive leaks and also for cases where autologus blood failed. Also consider bleb repair for repeated leaks or blebs that develop blebitis with associated leaks.

Dr. Barton, in cases of low IOP with corneal changes, does the IOP need to be raised prior to corneal transplant? How do you handle this given the view may be poor.
In cases of low IOP with corneal changes, corneal surgeons will often refuse to transplant unless the IOP is elevated.
If the view is poor, the principle is the same except you might have to take the tube out of the AC in order to thread the suture into the tube.

Can one do a scleral autograft where these other tissues are not available? That’s taking a partial scleral graft from the other eye?
When a scleral patch from an Eye Bank is not available, one can use sclera from the same eye, rotating a flap close to the original flap, and suturing it to the area that needs reduction of flow with 10-0 nylon. With this simple procedure, you don’t really need to remove sclera from the fellow eye.
If the cause of the hypotony after trabeculectomy (IOP is 5 mm Hg without athalamia after 1 month postop) is a cleft or a ciclodialysis in BMU with coroidal folds and low visual acuity what is your treatment approach? Oral Corticoides with mydriatics and topical corticoids and AINEs?
Excelent question. A cyclodialysis cleft can be treated initially with cycloplegics such as atropine. If this is not enough to close the cleft, argon or diode laser can be applied to both the sclera and the ciliary body using a goniolens. The idea is ti induce edema and inflammation, facilitating the closure of the cleft. If this is still insufficient, surgery may need to be done. In this case, one of the techniques that I use is to dissect a scleral flap over the cyclodialysis, expose the cleft and then suture the ciliary body to the sclera with 10-0 prolene. The scleral flap is then sutured with 10-0 nylon.

Dr Healey, what is the role of the manipulation of steroid dosage in the management of early hypotony?
The role of manipulation of steroid dosage in the management of early hypotony really depends on the reason for the hypotony and the likely scarring reaction of the patient. We know that the first 2 post-operative weeks are characterised by an infiltrate of the cells that subsequently activate, stimulate and preserve function of the fibroblasts responsible for scarring. The consequences of modulating steroid dosage in this period are seen in the severity of the scarring reaction many weeks later. While the modern paradigm of filtering surgery is to control flow with flap construction and control fibrosis with antifibrotics, in the pre-antifibrotic era, flow was the only mechanism to counter fibrosis and early overfiltration with choroidal effusions, shallow anterior chambers and poor vision were all considered necessary to ensure a satisfactory IOP months later.
The following scenarios may give you some guidance as to how to think about early (first 2 weeks) hypotony due to overfiltration post glaucoma filtering surgery.
1. Spontaneous improvement with standard post op therapy less likely. Reduction of steroid dosage more likely to be safe/helpful.
- Low/medium fibrosis risk with broad application of Mitmycin C, high flow trabeculectomy technique (small flap, large sclerostomy, loose sutures), high aqueous output, brief use of medical glaucoma therapy, minimal glaucoma therapy immediately pre-op, higher IOP target, chronic hypotony wth same technique in fellow eye, more concerning hypotony symptoms.
2. Spontaneous improvement with standard post op therapy more likely. Reduction of steroid dosage less likely to be safe/helpful.
- High fibrosis risk, no antifibrotic agent used, very low IOP target, Low aqueous output/ inflamatory glaucomas, prior failure of filtering surgery due to scarring, heavy aqueous suppression pre-op, chronic use of inflammatory/cicatricial/fibrotic glaucoma therapy, Asymptomatic (mild numerical) hypotony.
Do you bury the knot? The transconjuctival suture.
It is not necessary to bury knots when performing transconjunctival suturing. Just rotate them to sit flush against the surface. The ballooning conjunctiva sits will above the level of the knot and the patient will not feel any irritation.

Dr. Gedde, for eyes that develop cataract with hypotony, do you fix the hypotony first and then do the cataract? If you handle both at the same time, any tips for proper IOL selection?
In a patient with hypotony and cataract, I would recommend resolving the hypotony before proceeding with cataract extraction. We know the axial length can increase when IOP increases. If IOL calculations are performed using axial length measurements before the hypotony is addressed, cataract surgery may result in a subsequent myopic surprise. Additionally, keratometry readings may be unreliable in the setting of hypotony.
In eyes with higher risk of hypotony -esp young myopes- should a smaller plate size be used and can the plate be trimmed if late hypotony occurs?
I agree that a glaucoma drainage implant with a smaller end plate and/or a valved implant should be used in those patients who are at increased risk of hypotony. This includes patients with uveitic glaucoma, prior cyclodestruction, and advanced age. I do not believe that young myopes are at increased risk of hypotony after drainage implant surgery, but they are at higher risk of hypotony maculopathy should hypotony develop. Truncation of the end plate is one method that has been described to treat chronic hypotony after Baerveldt implantation.

Dr. Coleman, if low IOP causes choroidal effusions, do you drain them as part of the revision surgery?
It depends on how large they are. If they are outside of the peripheral arcade, I observe them since they will reabsorb with an increased eye pressure secondary to the revision.

WGA Society Spotlight
WGA Research Mentorship Program
The World Glaucoma Association (WGA) is proud to offer 3 places in their inaugural Research Mentorship Program in 2022. Developed by the members of the WGA Associate Advisory Board, which includes some of the top younger glaucoma researchers internationally, the program is designed to facilitate mentorship and nurturing of research skills in budding Ophthalmologists who wish to pursue glaucoma research and learn additional research skills.
Learn more: https://wga.one/wga/research-mentorship-program/

WGA Priority Point System
The World Glaucoma Association (WGA) offers several sponsorship opportunities for companies. With each sponsorship opportunity, a company earns a certain set of points. The WGA Glaucoma Industry Membership (GIM) program delivers most of the priority points. Other programs offered by the WGA provide additional points.
The WGA Priority Point Ranking is created to offer our loyal Glaucoma Industry Members priority handling to acquire their preferred sponsorship items and timeslots for the World Glaucoma Congress (WGC).
The WGA Priority Point Ranking applicable for WGC-2025 includes all points that were acquired during the last four years before the year in which the congress will take place. This means that for WGC-2025, a company’s priority points total is a sum-up of sponsorship contributions made in:
- 2021 (WGC-2021, Beyond Borders)
- 2022
- 2023 (WGC-2023, Rome)
- 2024
All WGA sponsorship programs confirmed before August 30, 2024, have been included in the 2025 ranking.
Should you have any questions related to the WGA Priority Points System, please contact the WGA Executive Office at info@worldglaucoma.org.
1. WGA Glaucoma Industry Membership
1.1. Glaucoma Industry Membership Level
Levels as of 2020
| Platinum Industry Members | 250 points |
| Gold Industry Members | 100 points |
| Silver Industry Members | 70 points |
| Bronze Industry Members | 17 points |
1.2. Seniority Glaucoma Industry Membership
10 points are awarded for each year of consecutive GIM support. Points are forfeited in the year consecutive GIM support ceases.
2. Fellowship Program
For each 1,000 USD spend on the Fellowship Program, a company receives 2 priority points.
5 points are awarded for each cycle of consecutive Fellowship Program support. Points are forfeited in the year consecutive Fellowship Program support ceases.
3. Education
3.1. Online Courses
Companies that support the development of 4 modules per year with 7,500 USD, receive 7,5 priority points.
3.2. Recorded sessions from past World Glaucoma Congresses
Companies that support the platform hosting the recorded sessions from past World Glaucoma Congresses for 7,500 USD per year, receive 7,5 priority points.
3.3. Meet the Glaucoma Expert Masterclass
Companies that support the development of the Meet the Glaucoma Expert Masterclass for 5,500 USD per year, receive 5,5 priority points.
3.4. WGA Global Webinar Series
Main sponsor
Companies that sponsor a WGA Global Webinar as the main sponsor, receive 1,5 priority points for each 1,000 USD spend.
Supporting sponsor
Companies that sponsor a WGA Global Webinar as a supporting sponsor, receive 1 priority point for each 1,000 USD spend.
4. International Glaucoma Review (IGR)
For each 1,000 USD spend on IGR advertisements, website banners, and newsletter banners, a company receives 2 priority points.
A company that signs an agreement for 1 volume, receives 5 additional priority points.
5. Journal of Glaucoma (JOG)
For each 1,000 USD spend on JOG sponsoring (as mentioned on page 30 of the WGA Industry Brochure), a company receives 2 priority points.
5 points are awarded for each year of consecutive JOG support. Points are forfeited in the year consecutive JOG support ceases.
6. World Glaucoma Week
For each 1,000 USD spend on WGW website banners and WGW newsletter banners, a company receives 1 priority point.
7. Communication
For each 1,000 USD spend on WGA website banners, WGA newsletter banners and advertising through social media, a company receives 1 priority point.
8. World Glaucoma Congress
8.1. Contribution to the previous two World Glaucoma Congresses
A. WGC Sponsorship Packages
| WGC Platinum Sponsor | 50 points |
| WGC Gold Sponsor | 30 points |
| WGC Silver Sponsor | 15 points |
| WGC Bronze Sponsor | 8,5 points |
| WGC Exhibitor | GIM | 3 points |
| WGC Exhibitor | non-GIM | 1,5 points |
8.2. Seniority Congress Sponsorship
- 5 points are awarded to companies that acquired a WGC Sponsorship Package or any other WGC sponsorship opportunity during one of the previous two congresses held (WGC-2019 & WGC-2021).
- 12 points are awarded to companies that consecutively acquired a WGC Sponsorship Package or any other WGC sponsorship opportunity during the previous two congresses held (WGC-2019 & WGC-2021).
WGA Patient Webinar: Lifestyle and Glaucoma
Can lifestyle changes help with your glaucoma? Exercise and a healthy diet are widely thought to benefit the body, including the eyes. To what extent do they actually affect the progression of glaucomatous damage to the optic nerve? In this 1-hour webinar for glaucoma patients and their loved ones, we explore the role of lifestyle, behavior, and diet on glaucoma with experts from all over the world.

WGA Patient Webinar
World Glaucoma Association – Patient Webinar
Can lifestyle changes help with your glaucoma? In this free 1-hour webinar for glaucoma patients and their loved ones, we explore the role of lifestyle, behavior, and diet on glaucoma with experts from all over the world.
For more information visit: https://wga.one/wga/patient-webinar/.
WGA Industry Brochure
WGA History
WGA is active and vital. It continues to develop and implement new programs for education and training.

WGA Global Webinar Recordings
This content is only accessible for logged-in users
WGA Global Webinar Recording Early Access
Thank you for joining the 9th Global Webinar: All About Minimally Invasive Glaucoma Surgery
As a registered participant, you have early access to the recording.
Download November 5, 2022 Program
👉 Log in to your WGA#One account to access previous webinars
WGA Finances

WGA Fellowships – Now and in the Future
Genetic testing will NOT be aimed at finding “the gene” for glaucoma rather it will be part of a glaucoma risk assessment for risk of disease onset, progression rate and response to therapy.

WGA Awards
WGA Awards were then offered. The Laureate Award was given to Roger Hitchings. The WGA Founders Award was given to Jeffrey Liebmann. Special Recognition Awards were to Jonathan Crowston, Chandra Sekhar Garudadri and Subhabrata Chakrabarti.

WGA 2024 Budget
Dear Governor,
We kindly request your approval for the WGA 2024 Budget.
Please submit your vote by Friday, April 12, 2024.
Should there be any questions, please do not hesitate to reach out to Liezl.botha@worldglaucoma.org.
Warm regards,
Ningli Wang, MD PhD
President,
World Glaucoma Association
Kaweh Mansouri, MD MPH
Executive Vice President,
World Glaucoma Association
WGA 2024 Association Financial Statement – Approval
Dear Executive Committee & Board members,
We kindly request your approval for the WGA 2024 Association Financial Statement.
Please submit your response by Friday, February 6, 2026.
Kind regards,
Arthur Sit
Treasurer
World Glaucoma Association
WGA – Funding Request
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login
Welcoming patients at the World Glaucoma Congress
Get the details of a successful patient symposium and outreach program at the WGC-2019.
At the World Glaucoma Congress 2019 in Melbourne Australia, host Josh Szeps sat down with Keith Martin (President WGA 2017-2019), Anne Brooks (President ANZGS), Shan Lin (Executive Vice President WGA) and Kaweh Mansouri (Associate Executive Vice President WGA) to talk about the World Glaucoma Association.

Welcome, introductions and meeting objectives

Welcome in Melbourne by Parliamentary Secretary for Health

Welcome in Helsinki
Minister Pirkko Mattila spoke on behalf of the Finish government

Welcome by WGA President

Welcome by Finnish Society
Hannu Uusitalo welcomed everybody on behalf of the Finish Glaucoma Society

Welcome and introduction
OAG is currently the main problem in the field of glaucoma and many patients are still undiagnosed.

Welcome & Introduction by WGA EVP

Wall of Fame
At every World Glaucoma Congress, we recognize and honor those who have significantly contributed to the success and positive development of the World Glaucoma Association, as well as the recipients of the ICO-World Glaucoma Association Three Month Fellowship Award.
A WGA Award recipient has been nominated by the WGA Executive Committee and presented for support to the WGA Board of Governors.
WGA Award recipients 2023
Laureate Award
Founders Award
Special Recoginition Award
WGA Award recipients 2021
- Laureate Award – George Spaeth (United States)
- Founders Award – Robert Ritch (United States)
- Founders Award – Tim Aung (Singapore)
- Special Recognition Award – Clement Tham (Hong Kong)
- Special Recognition Award – Kazuhisa Sugiyama (Japan)
- Fellowship Award – Yaseen Siddig Ahmed (Sudan)
- Fellowship Award – Nnubia Chinasa Anderline (Nigeria)
- Fellowship Award – Kintoki Makela GuyGuy (Congo)
- Fellowship Award – Aisha sheriff Kalambe (Nigeria)
- Fellowship Award – Evélia Marole (Mozambique)
- Fellowship Award – Meriem Seraj Nurrey (Ethiopia)
- Fellowship Award – Rebecah Nandasaba (Kenya)
- Fellowship Award – Ony Randrianjafisamindrakotroka (Madagascar)
- Fellowship Award – Diane Sonassa (Guinea)
- Fellowship Award – Arokoyo Oladele Vincent (Nigeria)
WGA Award recipients 2019
- Founders Award – Robert Fechtner (United States)
- Special Recognition Award – David Friedman (United States)
- Special Recognition Award – Peng Khaw (United Kingdom)
- Special Recognition Award – Olusola Olawoye (Nigeria)
- Special Recognition Award – Ki Ho Park (South Korea)
- Special Recognition Award – Norbert Pfeiffer (Germany)
- Special Recognition Award – Tarek Shaarawy (Switzerland)
- Fellowship Award – Bigirimana Deus (Burundi)
- Fellowship Award – Mohamed Elamin Abdelmoneim Elamin Mohamed (Sudan)
- Fellowship Award – Jagun Omodele Oluwayemisi (Nigeria)
- Fellowship Award – Lemlem Tamrat (Ethiopia)
- Fellowship Award – Faith Vata Masila (Kenya)
WGA Award recipients 2017
- Laureate Award – Roger Alan Hitchings (United Kingdom)
- Founders Award – Jeffrey M. Liebmann (United States)
- Special Recognition Award – Subhabrata Chakrabarti (India)
- Special Recognition Award – Jonathan G. Crowston (Australia)
- Special Recognition Award – Chandra Sekhar Garudadri (India)
- Fellowship Award – Farouk Garba (Nigeria)
- Fellowship Award – Philip Phatudi (South Africa)
- Fellowship Award – Martin Tchouyo (Cameroon)
WGA Award recipients 2015
- Founders Award – Franz Grehn (Germany)
- Special Recognition Award – Simon Bakker (the Netherlands)
- Special Recognition Award – Dennis Lam (Hong Kong)
- Special Recognition Award – George Lambrou (Greece)
- Special Recognition Award – Carlo Traverso (Italy)
WGA Award recipients 2013
- Founders Award – Makoto Araie (Japan)
- Founders Award – Kuldev Singh (United States)
- Special Recognition Award – Jian Ge (China)
- Special Recognition Award – Daniel E. Grigera (Argentina)
- Special Recognition Award – Robert Ritch (United States)
- Special Recognition Award – Mariska van der Veen (the Netherlands)
WGA Award recipients 2011
- Founders Award – Ivan Goldberg (Australia)
- Founders Award – Remo Susanna (Brazil)
WGA Award recipients 2009
- Founders Award – Erik Greve (the Netherlands)
- Founders Award – Roger Alan Hitchings (United Kingdom)
- Founders Award – Robert N. Weinreb (United States)
VS30 – Exchange of Ahmed Glaucoma Valve TM (AGV TM) in a Joint Tube in Persistent Plate Exposure
V. Pathak Ray, S. Dikshit
LV Prasad Eye Institute, Hyderabad, India
Purpose: To demonstrate the procedure of exchange of AGV from adult (FP7) to paediatric (FP8) model via a joint tube in persistent tube exposure.
Method/s and results: Video demonstration of the surgery, where patient had previous multiple attempts at closure, including the use of Conjunctival Auto-graft and Amniotic Membrane graft, and intake of Doxycycline.
Conclusion: It is possible to successfully manage recurrent plate exposure, with an exchange via a joint tube.

VS29 – Resolution of bilateral chronic hypotonous maculopathy following fortuitous management of bleb leak with autologous and h
V. Pathak Ray, R. Khanna, N. Chaudhuri, G. Sekhar
LV Prasad Eye Institute, Hyderabad, India
Purpose: To demonstrate the management of bilateral long-standing bleb leak with multiple origin donor tissue in a case of chronic hypotonous maculopathy.
Method: Video demonstration
Conclusion: Chronic bleb leaks with hypotonous maculopathy should be repaired, not only to reduce the risk of blebitis / endophthalmitis, but also for the resolution of the maculopathy and eventual visual rehabilitation.

VS28 – Amniotic membrane transplantation replacing absent conjunctival flap during phacotrabeculectomy
V. Castro, U. Zarate
Peruvian Glaucoma Society; Peruvian Ophthalmology Society
Unexpected intraoperative total dehiscence of conjunctival flap during phacotrabeculectomy and its replacement with lyophilized amniotic membrane graft is reported.
Adequate IOP control, deep anterior chamber and mild inflammatory conjunctival reaction was observed postoperatively. Although no bleb was seeing on biomicroscopy, positive Seidel sign was detected on third postoperative week; new amniotic membrane graft and two releasable sutures on scleral flap solved this complication.
Amniotic membrane graft was useful to solve challenging, intraoperative, total absence of conjunctival tissue.

VS27 – Pediatric glaucoma surgery- Watch out at each step!
S. Tejwani, J. Matalia, S. Dinakaran, K.B. Shetty
Narayana Nethralaya-, Bangalore, India
This video demonstrates the steps of most commonly performed surgery for pediatric glaucoma i.e. Trabeculectomy and trabeculotomy and also highlights the unexpected problems and their solutions at each step. In nutshell, it would serve as a guide to what precautions one should take at each step of surgery so as to avoid intra-operative complications and would also teach their management.
At the end, one can become confident of how to perform the
steps and what to anticipate at each level.

VS26 – Comparison of a valved & non-valved glaucoma drainage device, technique & outcome
S. Tejwani, S. Dinakaran, K.B. Shetty
Narayana Nethralaya-, Bangalore, India
This video demonstrates two cases to highlight the difference in the results of valved and non-valved shunt devices. First case of valved shunt presented with advanced glaucoma and pseudophakia after a difficult cataract surgery and failed filtration surgery. Second case of non-valved shunt, was an aphakic glaucoma with
failed filtration surgery & eccentric pupil in the only seeing eye. Both the patients had good IOP control in the long term however the non-valved shunt had a longer hypertensive phase.

VS25 – Learn from yesterday, live for today, hope for tomorrow
S. Banerjee, D. Pal, R. Choudhary Ramakrishna Mission Seva Pratishthan, V.I.M.S., W.B., India; M.P. Birla Eye Foundation, W.B., India; Disha Eye Hospitals, W.B., India
46 Yrs lady rushed into clinic with complaints of painful gross diminution in vision for last 48 hours in her only seeing eye with watering and blepharospasm. The fellow was post injury phthisical.
Detailed examination revealed a leaking trabeculectomy bleb, flat to nil AC, clear cornea and intumuscent Cataract. Vision was accurate ray projection only and IOP 4 mmHg.
This video shows bleb repair by autologous scleral patch graft and simultaneous phaco with PC-IOL and most amazing post-op visual recovery.

VS24 – Malignant glaucoma: Can it be benign?
S. Dikshit, S. Senthil, C.S. Garudadri
LV Prasad Eye Institute, Hyderabad, India
A shallow or flat anterior chamber characterizes malignant glaucoma in the presence of patent iridotomy usually with high intraocular pressure, following an intraocular surgery. The condition is severe and progresses relentlessly and hence the name. Diagnosis and management of this condition is a big challenge. In this video we demonstrate a simple approach to diagnose malignant glaucoma
and also present a stepladder approach for the management of malignant glaucoma.

VS23 – Trabeculectomy with suprachoroidal derivation
R. A. Perez Grossman, D. Grigera, A. Wenger
Instituto de Glaucoma y Catarata, Lima, Peru
We present a novel glaucoma surgery for patients with secondary open angle glaucoma and refractory glaucoma, a trabeculectomy with Mitomycin C and suprachoroidal derivation. We create an intrascleral tunnel using 2 flap of autologous sclera that will direct the aqueous humor from the anterior chamber to the uprachoroidal space, having the advantage of using 2 different drainage pathways to lower the IOP, the anterior chamber to subconjunctival space fistula and the uveoescleral drainage through the suprachoroidal space.

VS22 – Phacomorphic glaucoma in nanophthalmos
J.J.Praveen, N. Choudhari, R.K. Reddy, G.Chandra Sekhar
LV Prasad Eye Institute, Hyderabad, India
Multiple quadrant prophylactic sclerotomy is believed to prevent uveal effusion associated with intraocular surgery in nanophthalmic eyes.
This video shows phacoemulsification surgery in the management of phacomorphic glaucoma in a nanophthalmic eye. Two radial sclerotomies could not prevent intraoperative suprachoroidal effusion.
The learning points are discussed. A secondary intraocular lens insertion was uneventful.

VS21 – Implantable Collamer Lens (ICL) explantation with trabeculectomy
J.J. Praveen, S. Senthil, P.K. Vaddavalli
LV Prasad Eye Institute, Hyderabad, India
A 24-year-old, with a best-corrected vision of 20/20, developed secondary glaucoma following a fulminant course of post operative inflammation after Posterior Chamber Implantable Collamer Lens implantation (ICL) for correction of high myopia. The medically uncontrolled intraocular pressure necessitated explanation
of ICL combined with trabeculectomy. Glaucoma though rare, is a vision threatening complication following ICL implantation. In this video we demonstrate the management of this serious sight threatening complication.

VS20 – Where does the aqueous go?
M. Coote
Royal Victorian Eye and Ear Hospital, Melbourne, Australia; Glaucoma Surgical Research Unit – Centre for Eye Research Australia (CERA), Melbourne, Australia
Following successful trabeculectomy it is assumed that most aqueous enters the bleb and is absorbed by capillaries in the bleb. But it is not clear whether aqueous enters the cut ends of Schlemm’s canal. In this video an unusual aqueous vein developed after glaucoma surgery in a PDG eye and aqueous can be seen to (repeatedly) ‘burp’ through it following brief IOP elevation. It strongly suggests that, at least sometimes, trabeculectomy functions in the way that Cairns proposed.

VS19 – Releasable suture – Reining the horse
M. Khamar1, D. Agrawal1
Raghudeep Eye Clinic, Ahmedabad, India
Trabeculectomy aims at a steady aqueous flow. Maintaining the right amount of flow is a challenge. Very tight sutures can result in reducing aqueous outflow causing bleb failure. Very loose sutures will result in overfiltration and hypotony. Therefore titration of filtration in early postoperative period is important.
Releasable suture regulates the aqueous outflow. It has an advantage over suturolysis, as visualization is not difficult , easy to remove and does not require laser.

VS18 – Clinical application of anterior segment optical coherence tomography associated with glaucoma surgery
K.S. Lee, K.H. Songh, J.R. Lee, K.R. Sung
Department of Ophthalmology, University of Ulsan, College of Medicine, Asan Medical Center, Seoul, South Korea
Anterior segment optical coherence tomography (AS-OCT) is becoming a useful diagnostic modality in the glaucoma field. AS-OCT has the advantage that images can be obtained in the sitting position using a non-contact method, which is extremely helpful in the evaluation of perioperative conditions. In this film, we intend to show the creative clinical applications of AS-OCT in various glaucoma surgical procedures. We demonstrate several clinical cases where AS-OCT is used as a helpful procedure in pre- and post-operative glaucoma patients.

VS17 – Ahmed glaucoma valve(TM) (AGVTM) implantation in iridocorneal endothelial syndrome
K. Ravi, N. Choudhari, B.L. Harsha
LV Prasad Eye Institute, Hyderabad, India
The proliferating abnormal endothelial cell layer may hypothetically close the ostium and thereby reduce the success rate of trabeculectomy in Irido Corneal Endothelial (ICE) syndrome. This video demonstrates implantation of Ahmed glaucoma valve as the primary anti-glaucoma surgery in an eye with ICE syndrome and
related difficulties. In addition, we did encounter wound dehiscence in the early post-operative period. The video also shows successful conservative management of the complication by addition of oral Doxycycline to the post-operative regimen.

VS16 – Exfoliation and pseudoexfoliation: not “two of a kind”
J.C. Mesa-Gutiérrez, J. Hoyos-Chacón, A. Rouras López
Hospital Esperit Sant, Barcelona, Spain
We present a rare case of true exfoliation as an incidental finding in a phaco surgery of a white cataract. A first but troublesome continuous circular capsulorrhexis (CCC) was performed. Hydrodisection was attempted but was not possible, so diagnosis of true exfoliation was suggested proceeding to a second and successful CCC. A biopsy of anterior capsule revealed true delamination. Pictures of the lens of the fellow eye, both optic discs and optical coherence tomography were taken to rule out pseudoexfoliation.

VS15 – Tectonic scleral autograft for treatment of Mitomycin C scleral melting
J.C. Mesa-Gutiérrez, J. Hoyos-Chacón, A. Rouras López
Hospital Esperit Sant, Barcelona, Spain
We present a technique for treating scleral melting secondary to Mitomycin-C in a previous deep sclerectomy (DS). A scleral graft with tectonic function was used.
A partial thickness scleral graft was harvested using a 2 mm dermathological punch. Melted sclera was excised with the same punch and the original DS flap sutured to the scleral graft. A double conjunctival flap covered the scleral graft. Hypotony was solved and a functioning bleb after 18 months follow-up was observed.

VS14 – Ahmed glaucoma valve: Innovations in wound closure with fibrin glue
J. Shah, L. Vijaya
SMT Jadhavbai Nathmal Singhvi Glaucoma Services Sankara Nethralaya, Chennai, India
Ahmed glaucoma valve has been the mainstay of surgical treatment in cases of refractory glaucoma. The tube is usually covered by a piece of donor sclera or cornea. Donor tissue anchorage and conjunctival closure is done usually with non-absorbable nylon or absorbable vicryl sutures.
In this video, we have demonstrated the use of fibrin glue instead of sutures, and highlighted the advantages and disadvantages of the same.

VS13 – Challenge of the tube
G.A. Lee
City Eye Centre, Brisbane, Australia
Aim: To describe the surgical management of a Baerveldt tube causing corneal decompensation
Methods: Video presentation of surgical procedure and post-operative outcome.
Results: The tube of the Baerveldt was exposed and tied off with 7/0 vicryl. The tube was explanted from the anterior chamber and repositioned using a McCannell suture to pass under the iris into the sulcus, anterior to the intraocular lens. The tube was covered with a full-thickness scleral patch graft. An endothelial keratoplasty
using a Descemet stripping technique (DSEK) was performed, inserting a 9.0mm graft, via a Busin glide. An air bubble was placed in the anterior chamber and the patient positioned face up for 48 hours. The vicryl tie was removed at 7 days to allow the tube to drain and restore normal intraocular pressure.
Conclusions: This video presents an approach to a complex anterior segment and glaucoma problem. By using lamellar grafting techniques and managing the intraocular pressure carefully post-operatively, the most rapid rehabilitation of vision can be obtained, with longer term stability of the cornea and glaucoma
control.

VS12 – Tube repositioning in anterior chamber in tube related complications of aqueous drainage devices
G.V. Puthuran, R. Kapa, R.R. Krishnadas, A.L. Robin
Glaucoma Society of India, Aravind Eye Hospital, Madurai, India, American Glaucoma Society
Aqueous drainage devices play an important role in treatment of refractory glaucomas.Inspite of meticulous tube placement and surgical closure tube cornea contact, tube retractions occur necessitating removal of tube and reinsertion via a new sclerotomy. Surgeons occasionally need to lengthen the tube to effectively
manage tube retractions.The tube extender is a useful,commercially available device when the tubes of glaucoma drainage implants from different manufacturers require lengthening.

VS11 – Evolution of an affordable aqueous drainage implant – The Indian Story
G.V. Puthuran, P. Palmberg, A.L. Robin, S. Parthasarathy, R. Kapa, S.R. Krishnadas
Glaucoma Society of India, Aravind Eye Hospital, Madurai, India, American Glaucoma Society
All modern glaucoma drainage implants are cost prohibitive for poor populations. The Aurolab Aqueous Drainage Implant (AADI) is a non-valved aqueous shunt made of Nusil permanent implant silicone elastomer which has passed tissue culture cytotoxicity testing. It’s design is greatly influenced by the original Baerveldt
glaucoma implant 350. The AADI is a low cost alternative for patients with refractory glaucoma in resource poor communities in the developing world.

VS10 – Ultrasonic circular cyclo-coagulation in a patient with primary open-angle glaucoma
F. Aptel
Joseph Fourier University, Grenoble, France; Department of Ophthalmology, University Hospital of Grenoble, Grenoble, France
We have developed a ring-shaped device allowing to selectively coagulate the ciliary body with high-intensity focused ultrasound. We present a procedure in one patient having primary open-angle glaucoma, and then discuss the first clinical results and the mechanisms of action of this new method.

VS09 – Blocking the tube with vicryl…breaking a vicious cycle
D. Pal, A. Chatterjee, J. Sengupta
Aravind Eye Care System, Priyamvada Birla Aravind Eye Hospital,Kolkata, India
72 yrs hypertensive gentleman with intractable post-PK glaucoma presented with profound visual loss following Ahmed Glaucoma Valve implantation on the 4th post operative day with an IOP of 4. USG revealed increasing hemorrhagic choroidal detachment. Drainage of the choroidal fluid was combined with blocking the valve lumen using 6-0 vicryl suture. The IOP increased slowly and the choroidals settled over next 2 weeks. The vicryl suture got dissolved by 5th week, IOP became normal and vision improved gradually.

VS08 – Manual small incision cataract surgery in a case of phacolytic glaucoma
D. Pal
Aravind Eye Care System, Priyamvada Birla Aravind Eye Hospital, Kolkata, India
57 yrs old lady presented with painful red eye, high IOP, light perception vision and hypermature cataract. A prompt diagnosis of phacolytic glaucoma was made. Manual small incision cataract surgery was performed with placement of a 3piece PMMA IOL. Intra-operative zonular dehiscence was managed by endocapsular
ring insertion.

VS07 – Re-implantation of Ahmed glaucoma valveTM (AGVTM) in a case of AGVTM extrusion
A.K. Roy, S. Senthil
VST Glaucoma Centre, L V Prasad Eye Institute, Hyderabad, India
It is challenging to implant Glaucoma Drainage Devices (GDD) in the management of refractory glaucomas with extreme conjunctival scarring from multiple intraocular procedures. We present the implantation procedure in a case of severely scarred conjunctiva in a 45 year old, one-eyed, aphakic, highly myopic female. This was a successful implantation of inferior Ahmed™ Glaucoma Valve (AGV™) with primary scleral patch graft and conjunctival autograft, status post vitreoretinal surgery for retinal detachment with an extruded AGV™ in the superior quadrant.

VS06 – Management of congenital glaucoma associated with stickler syndrome
A.K. Mandal, B.H. Shenoy
L. V. Prased Eye Institute, Hyderabad, India
Stickler syndrome with Pierre Robin Sequence and bilateral congenital glaucoma is a rare disease. Present video highlights the management of such a child of one month age. Simultaneous bilateral primary combined trabeculotomy with trabeculectomy were performed under general anesthesia. The child’s surgery was successful in controlling intraocular pressure, restoring corneal transparency, but required spectacle correction of -16.00 Dsph in both eyes. There were no intra-operative and postoperative complications. A multidisciplinary approach was required for the successful management of this child.

VS05 – Glaucoma in phacomatosis pigmentovascularis
A.K. Mandal
L. V. Prased Eye Institute, Hyderabad, India
Glaucoma in Phacomatosis Pigmentovascularisis (PPV) is challenging. The present video highlights the surgical technique of primary combined Trabeculotomy and Trabeculectomy (CTT) on both the eyes of a two month old child with PPV. Forty eyes of 24 children with various types of PPV were managed by a single surgeon over a period of 20 years (1990 -2010). Intraocular pressure control is satisfactory with cumulative success probability of 93% at 66 months follow-up. However, visual outcome is sub-optimal.

VS04 – Combined cataract and trabeculectomy in subluxated cataracts
B. Ganguly, D. Pal
Aravind Eye Care System, Priyamvada Birla Aravind Eye Hospital,Kolkata, India
A 52 yr old geltleman presented with uncontrolled poag and associated subluxated hard cataract.he underwent small incision (manual)cataract surgery with ctr and iol implantation with trabeculectomy
with mitomycin-c and had 6/12 bcva and well controlled iop in 1 year of follow up.
the next patient was a 37 yr male who had a spontaneously subluxated lens with poag and underwent trabeculectomy with mitomycin-c and iris fixated iol implantation and had good visual recovery and iop control for 17months follow up.

VS03 – Lost and found – Ahmed glaucoma valve during implantation
A. Ganguly, D. Pal
Aravind Eye Care System, Priyamvada Birla Aravind Eye Hospital,Kolkata, India
A 30 yrs old male patient a case of pseudophakic juvenile glaucoma a repeat trabeculectomy failure with maximal medical therapy underwent an ahmed glaucoma valve implantation. during implantation the ahmed glaucoma valve slipped behind the equator of the globe and was eventually recovered by careful retaction of
the conjuctiva and the tenon’s capsule. this video demonstrates the do’s and don’t’s during such an eventuality and the sucessful completion of the case.

VS02 – Deep sclerectomy with insertion of a prolene 5/0 segment inside Schlemm’s canal
A.M. Abdelrahman
Cairo University, Giza, Egypt
The film shows a novel technique of manual insertion of a 12-mm 5/0 Prolene thread inside Schlemm’s Canal (SC). Deep Sclerectomy is initially performed, and then a Prolene suture is inserted through both Ostia of SC, leaving the middle portion of the thread crossing the Trabeculo- Descemet’s membrane (TDM). The thread is expected to prevent SC collapse and allow visualization of the thread through the TDM in case goniopuncture is needed, beside the low cost of the implanted Prolene.

VS01 – Non-technical skills for eye surgery
B. Mohamed, A. Azuara Blanco, E. Henderson
Queen’s University Belfast, Institute of Clinical Science, Royal Victoria Hospital, Belfast, United Kingdom
Safe an efficient surgery requires more skills than good technique. Surgical errors in ophthalmology can often be directly or indirectly associated with the lack on non-technical skills such as communication,
awareness, leadership and decision-making.
The purpose of this film is to emphasize the importance of non-technical skills in ophthalmic surgery and show the possible consequences of lacking non-technical skills on patients and the team. Different scenarios are simulated.

Vote of the General Assembly of Glaucoma Societies
Vote of the General Assembly – WGA Board of Governors
Vit B (Niacin) for the treatment of glaucoma – too good to be true?
Jonathan Crowston introduces the reasons why Vit B3 may serve as a glaucoma therapeutic option because of its impact on the bioenergetic deficiency associated with ageing. Older age is associated with greater risk of developing POAG and Prof Crowston lists the associations with Mitochondrial dysfunction and reduced NAD+ reduced with age as possible contributory factors. The high energy requirements of neuronal tissue could explain this decline with age. Since RGC’s are very long and partly myelinated there may be different energy requirements in different portions with corresponding susceptibility. He presents evidence from clinical POAG and LHON cohorts that demonstrate an association with mitochondrial dysfunction seen as complex I abnormality especially with age. The reasons for NAD + decrease with age are discussed. He presents data from animal experiments that have demonstrated that Niacin modulated mitochondrial dysfunction prevented glaucoma in an inherited mice model for glaucoma even at low doses.

Visual impairment and reading performance

Visual Fields are Best for Managing Glaucoma Suspects
It is accepted that OCT is the standard in monitoring for early progression in glaucoma. Visual field testing however also plays an important role in suspects or early glaucoma patients. Literature exists on evidence of VF changes in early glaucoma (including early changes noted on central visual field testing). OCT artifact can make interpretation difficult and visual field testing can provide functional information that OCT can not.
From the Education Committee
Dr Albert Khouri started saying that he would try to convince us to do both: structure and functional analysis in glaucoma. The best test for one patient depends on the stage of the disease. In the very beginning the visual field would not help us, but the retinal nerve fiber layer thickness could. He said that nowadays we know that we have damage in central field in glaucoma even in early stages. He presented a research that RNFL thickness detected progression as well as visual field. And looking at this particular study, visual field and OCT were done in every single visit. He emphases that not every red in OCT is a real disease, some cases such as tilted disc or peripapillary atrophy may be challenging for OCT and in these cases visual field by help us. He said that in EMGS, visual field was very helpful to detect progression. Finally, visual field can be very useful even in the early process.

Visual fields and prediction of visual loss in glaucoma
Big data is extremely large data sets that may be analyzed computationally to reveal patterns, trends, and associations that relate especially to human behavior and interactions. Do we have the big data about glaucoma?
Detecting glaucoma requires a thorough analysis along with a relevant examination of risk factors and changes in structure and function. Dr. Tatham lectures about the specificity and sensitivity as well as the strengths and limitations of these tests. Access to modern technology in low income countries is challenging but the necessity for diagnosis, documentation and follow-up supersedes these challenges because the rate of blindness and advanced glaucoma are becoming more frequent. Dr. Philippin shows how to use smartphone cameras, low cost ophthalmoscopes as well as how to conduct visual field tests with a laptop in underdeveloped areas.
Open angle glaucoma has a significant genetic component with a relative risk of over 9 in first-degree relatives of affected individuals when compared to relatives of unaffected people. Genome-wide association studies (GWAS) have now successfully identified important genetic variants associated with many human traits and diseases. Dr. Hewitt introduces us to this innovative and groundbreaking topic. After, Dr. Craig addresses interactions between genes and their environments with valuable examples about the upregulation of the myocilin gene with steroids and the increased expression of LOXL1 under UV irradiation in Pseudoexfoliation.
What information enables an analysis of half million of the visual field? David Crabb provides data of VF progression, the initial presentation stage of glaucoma, and the right frequency of testing that may surprise you as well as save costs in the health care system.

Visual fields
Ananth Viswanathan gave the second presentation in which he focused on the visual field. He mentioned that there were basically 4 domains to getting the most out of visual fields: infrastructure, technical staff, clinical staff and patients. He mentioned that 6 visual fields were necessary in the first 2 years for newly diagnosed manifest glaucoma. He stressed the need for properly trained technical staff and guidelines/protocol/standard operating procedure to guide the staff. He also mentioned that visual field progression can be assessed based on event (GPA) analysis and trend (progressor) analysis. He concluded that it was important for patients to be properly counselled on how to do the visual field test to get the best and most reliable result.

Visual field testing in natural environments

Visual Crowding in Glaucoma

Visual Crowding in Glaucoma
In glaucoma patients, a pronounced visual crowding effect is observed, even in the presence of mild visual field loss on standard perimetry. The severity of visual crowding was associated with the amount of neural loss quantified by optical coherence tomography. These results may have implications for understanding how glaucoma patients are affected in daily tasks where crowding effects may be significant, such as driving, reading, visual search, and object identification.
In glaucoma patients, a pronounced visual crowding effect is observed, even in the presence of mild visual field loss on standard perimetry. The severity of visual crowding was associated with the amount of neural loss quantified by optical coherence tomography. These results may have implications for understanding how glaucoma patients are affected in daily tasks where crowding effects may be significant, such as driving, reading, visual search, and object identification.

Visual Assistive Equipment

Vision-Related Quality of Life in Glaucoma

Vision of EGS

Visco-BANG: MIGS for All
We demonstrate a variation of the Bent Ab Interno Needle Goniectomy, which is performed with a 30 G needle mounted on a syringe of Viscocohesive agent. The needle is engaged in the Schlemm’s canal, followed by viscodilation and goniectomy.
Dr Anin Sethi (Dr Agarwals Eye Hospital, Chandigarh, India) Dr Nitika Beri (Department of Ophthalmology, University College of Medical Sciences, Delhi, India) Dr Tanuj Dada (Dr Rajendra Prasad Centre for Ophthalmic Sciences, A.I.I.M.S., New Delhi, India)

Virtual WGA Symposium at APGC 2022
Bleb and Non-Bleb Based Surgeries: Pearls from International Experts
Join the virtual WGA Symposium on Bleb and Non-Bleb Based Surgeries: Pearls from International Experts taking place during the Asia-Pacific Glaucoma Congress on August 4, 2022, from 1:00-2:30 PM Malaysia Time (Find your local time here).
Program
1. Introduction – Neeru Gupta, MD PhD MBA
2. Welcome & Introduction by the moderators – Kaweh Mansouri, MD & Tanuj Dada, MD
3. Micropulse TLT: Clinical Pearls for the Best Results – José Maria Martinez de la Casa, MD
4. Canaloplasty or Goniotomy: Which is best? – Inder Paul Singh, MD
5. Stenting: How to make them work for the patient – Kyung Rim Sung, MD
6. XEN: Inside Out vs. Outside In – Kaweh Mansouri, MD
7. TRABS: Best practices for successful outcomes – Paul Healey, MD
8. Tubes: Optimizing your outcomes – Da Wen Lu, MD
9. Panel discussion – All moderators & speakers
For registration visit: https://apgcongress.org/.
Virtual glaucoma clinics
A streamlined glaucoma service can provide safe and cost-effective care, when an optometrist is supported by an ophthalmologist via web-based virtual oversight.

Virtual Glaucoma Clinic

VII PERUVIAN GLAUCOMA CONGRESS
Join the Peruvian Society of Opthalmology for their Peruvian Glaucoma Congress on the 10 through 12 April 2025.
The Peruvian Society of Opthalmology is a non-profit scientific institution that brings together Ophthalmologists and Ophthalmology Residents for Academic purposes.
Find out more here.
Video Submission Terms & Conditions
BY SUBMITTING THE VIDEO, IMAGES, SOUNDS AND/OR LIVE-STREAM (COLLECTIVELY, “VIDEO CONTENT”) YOU ARE ABOUT TO SUBMIT, YOU AGREE TO BE BOUND BY THESE TERMS AND CONDITIONS (“SUBMISSION TERMS”).
By submitting the Video Content you retain full copyright of the Video Content. You grant the World Glaucoma Association (“the WGA”) and its assignees, licensees, successors in interest, legal representatives and heirs the right to use, distribute, transmit, stream, broadcast, publicly perform, reference, store, cache, and otherwise utilize (including through its communication channels) the Video Content for educational, promotional and marketing purposes. You hereby waive any right to inspect or approve the Video Content or printed or electronic matter that may be used in conjunction with such content now or in the future and you waive any right to royalties or other compensation arising from or related to the use of the Video Content. You also grant the WGA the right to use your first name, last name, and country in connection with the Video Content, although the WGA will have no obligation to use your name or credit you in any way in its use of the Video Content.
You hereby make all warranties, representations and guarantees with respect to the Video Content that you submitted with respect to the Video Content as defined in the Checklist for submission, including but not limited to a representation and warranty that the Video Content does not infringe or violate the intellectual property rights or proprietary rights, rights of publicity or privacy, or other rights of any third party. In addition, you represent and warrant that you have received and will maintain the necessary consents, permissions and approvals from anyone who appears in or is heard in any of your Video Content, including without limitation (1) permission for their image and/or voice to appear in that Video Content and (2) permission for that Video Content to be submitted to us pursuant to these Submission Terms.
By clicking I Agree, you represent and warrant that you have full power and authority to agree to these Submission Terms, including without limitation the power and authority to grant all rights relating to the Video Content. It is at the discretion of the WGA to decide whether and how to use the Video Content. The WGA claims no ownership of your Video Content.
Video library search
Video Library
Viable Glaucoma Therapy in the Developing World

VGI in special case (post vitrectomy and silicone oil)

VGI in East Java

Vasculomics: Novel imaging modalities for dynamic ocular blood flow

Vascular dysfunction and NTG – myth or reality

Vascular Changes in Experimental Glaucoma

Vascular Biomarkers in Glaucoma: from 24 hour ocular perfusion pressure to OCT angiography
Risk factors for glaucoma can be differentiated from biomarkers. Conventional biomarkers in glaucoma diagnostics are structural measures such as C/D ration, RNFL thickness, stereometric parameters, and functional measures (VF).
Vascular biomarker (e.g. vessel density, FAZ related parameters) might be of importance in detection of glaucoma.

Valved drainage devices

Valved and non-valved glaucoma drainage devices

Uveitis and glaucoma
Anthony Hall, a uveitis expert from Melbourne, discussed the epidemiology, etiology, and treatment options in uveitic glaucoma. Data are reviewed showing that roughly 20-30% of patients followed for uveitis clinic will present with significant IOP elevation after 10 years of follow-up, with particularly high rates of associated glaucoma in eyes with uveitis due to Posner-Schlossman, viral infections, toxoplasmosis, and JIA. In one study, even higher rates of glaucoma were noted, with 6% of eyes developing glaucoma annually, and nearly 2% of eyes going blind from glaucoma annually. Dr. Hall describes the various mechanisms of glaucoma in uveitis, broadly dividing mechanisms into open vs. closed angle mechanisms. Steroid response also plays a role in uveitic glaucoma, and data are reviewed suggesting that with enough steroids, most patients will demonstrate an IOP rise. Regarding the management of glaucoma, caution should be given to OCT imaging, as uveitis can be associated with RNFL thickening. Regarding treatment, Dr. Hall emphasizes that proper treatment of the inflammation is critical, and suggests that fears regarding prostaglandin therapy are overblown. He also reviews the broad array of surgical treatments, including trabeculectomy and tube shunt surgery.

Uveitic Glaucoma

Uveitic
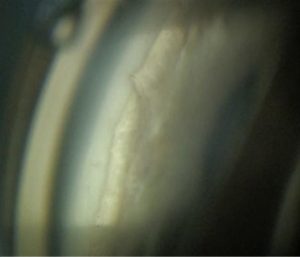
Using OCT to assess Retinal Oxygenation- implications for Glaucoma Specialists

Using genetics to customize the choice and timing of surgery

Using AI to find early cases of glaucoma

Using AI in Glaucoma Imaging

User Account – New
User Account
User Account – New
User Account
Usefulness of OCT angiography in glaucoma diagnosis and management
OCTA is an attractive technology and can provide additional useful information in glaucoma diagnosis and management.

Usefulness of OCT angiography for early glaucoma

Useful Science Under Pressure

Use of Collagen Matrix versus Mitomycin C in Primary Trabeculectomy: Experience in the West Indies

Use of Anterior Segment Imaging in MIGS

Urrets-Zavalia after GATT

Update on Uveitic Glaucoma

Update on Optic Nerve Regeneration

Update on New Glaucoma Implants

Update of MIGS in Bangladesh

Update Glaucoma Societies
Rob Fechtner announced new societies members of the WGA, and thanked the Industry members of WGA.

Unusual case of pupillary block sixteen years after phacoemulsification: A Diagnostic challenge!
Meticulous clinical examination augmented by ultrasound biomicroscopy helped in diagnosing and managing this case for satisfactory intraocular pressure and visual outcome.

Unmet needs in Surgical Therapy

Unmet needs in Medical treatment

Unmasking silicone oil-filled anterior chamber
Diagnosing silicone oil-filled anterior chamber can sometimes be challenging due to the absence of classic pupillary block indicators.Three major signs indicative of the presence of silicone oil-filled anterior chamber and its treatment is elucidated
1. Dr.Sahiti Puttagunta – Fellow in glaucoma, LVPEI, Hyderabad, India 2. Dr.Pratinya Kolipaka – Glaucoma consultant, LVPEI, Hyderabad, India 3. Dr.Rashmi Krishnamurthy – Glaucoma consultant, LVPEI, Hyderabad, India 4. Dr.Sirisha Senthil – Head of glaucoma services, LVPEI, Hyderabad, India

United Kingdom & Eire Glaucoma Society (UKEGS) Annual Meeting 2022
United Kingdom & Eire Glaucoma Society (UKEGS) Annual Meeting 2022
UK & Eire Glaucoma Society – UKEGS goes live! The next UKEGS Conference will be a face to face meeting on 21 and 22 April 2022, hosted by UKEGS President Prof Pete Shah at the IET Austin Court in central Birmingham.
For more information, visit: https://glaucoma.uk/ukegs/.
Unilateral Open Angle Glaucoma in an Adult with Large Corneas

Understanding surgical augmentation of suprachoroidal outflow in the era of MIGS and Interventional Glaucoma
Suprachoroidal MIGS Surgery is an interesting surgical option for glaucoma.
Postop. IOP is not limited by episcleral pressure.
It is worth to explore as it has potencial to treat more advanced cases.
But:
1.- IOP decrease is limited by scarring/encapsulation. Difficult to manage.
2.- Have to refine improve the surgical procedures, however new materials and design could improve the safety profile.

Understanding simple and complex statistics in research publications
Engage a biostatistician before and during study design
Collect preliminary data
Do your own analysis
Spend time determining the frequency, distribution (binomial, ordinal, normal, etc….), and shape (Kurtosis, right skewed, left skewed)
Look for outliers, miscoded data, etc….
Results should make clinical sense
From the Education Committee
Dr. Steve Mansberger opens the session, discussing, in a quiz format, several basic statistical flaws in manuscripts that are submitted for publication, and explains key concepts worth brushing up for more critical reading of published work. This talk is relevant for both author and reader of “statistically spiced” research.

Under Pressure: Making surgical decisions

Uncontrolled IOP in JOAG: Trabeculectomy

Uncontrolled IOP in JOAG: MIGS

UK biobank: lessons from a 100,000 person cohort study
Development of UK BioBank offers novel insights into eye disease in the UK and worldwide.
From the Education Committee
Dr. Paul Foster highlighted the importance of UK Biobank, one of the world’s largest ophthalmic datasets comprising 503,000 participants from 22 recruitment centers in the UK, in affording mechanistic insights into glaucoma and other eye diseases. Some of the interesting discoveries from the UK Biobank include intraocular pressure-lowering effect of vitamin C, association between retinal pigment epithelium thickness and intraocular pressure, and development of genetic prediction models for primary open-angle glaucoma.

UK & Eire Glaucoma Society Conference 2025
The UK and Éire Glaucoma Society invites you to there 2025 Congress taking place 5th to 6th November.
Find out more here.
Type of anesthesia and changes in anticoagulation therapy

Turning stem cells into retinal ganglion cells: A translational model of neurodegeneration and human disease pathology

Tubes: who, when & why?

Tubes, Mitomycin & Microfluidics

Tubes with Boston KPro – Where do i put it & how do I monitor?

Tubes management for refractory glaucoma

Tubes in challenging cases: how to manage the success

Tubes and cyclophotocoagulation

Tubes & cyclophotocoagulation

Tubes

Tube surgery: Does size or valved matter?
Dr Brandt described the indications of tube in pediatric glaucoma and also reviewed the literature on the outcomes of pediatric tube surgery. He also reviewed the literature on the use of anti-fibrotic agents in pediatric tube surgeries. He then summarized the different valved and non-valved drainage devices, discussing the advantages and disadvantages of each of them. Finally, he went over the steps of the pediatric tube surgery in detail highlighting the precautions required in each step to avoid complications.

Tube location and sealing methods
This content is restricted and only accessible to WGC-2019 participants
Login

Tube implant in an eye with staphyloma

Tube has failed, what next?

Tube exposure
Special attention must be paid to risk factors. The first sign (thinning of the patch) should be carefully followed. When there is exposure, both the site and its surroundings should be assessed. Different options for repair are illustrated, according to the findings. Observation of bacterial plaques represents urgency. The decision of the technique to be applied must be made following the five-step algorythm that is presented. Use the surgical option that best suits your case. Remember, nothing lasts forever!
From the Education Committee
Daniel Grigera dealt with tube exposure and reviewed the literature regarding risk factors for the exposure. He gave different management options depending in the degree and location of the exposure and whether there was co-existent infections. He described various surgical options including transposition of the conjunctiva and repositioning of the tube based on etiology.

True exfoliation syndrome reawakened
True exfoliation or capsular delamination was initially described in workers affected by high heat. Dr Teekhasaenee describes this uncommonly reported and also benign condition.

Trends in Utilization of Laser and Incisional Glaucoma Surgeries Performed on Medicare Enrollees by Glaucoma Specialists Versus Non-Specialists from 2008-2016
An increasing trend was seen in the number of Medicare beneficiaries undergoing glaucoma surgery between 2008-2016. Trabeculectomies showed a downward trend while drainage device implantation and Minimally invasive glaucoma surgery(MIGS) were on an upward course. Nearly three quarters of these surgeries were performed by trained glaucoma specialists.

Trends in Prevalence / Burden

Treatment strategies for Uveitic glaucoma and UGH syndrome

Traumatic Glaucoma Update

Translating Blood Flow Research into Clinical Practice

Translaminar pressure gradient and glaucoma
These forces cause the tissue distortion and compression along with axonal and blood flow changes pivotal to glaucoma. How the gradients change in glaucoma progression informs our understanding of disease stability with treatment.
From the Education Committee
Intraocular pressure (IOP) alone does not explain why some patients develop glaucoma or continue to progress despite treatment. Dr. Bill Morgan discusses the importance of translaminar pressure gradient, dependent upon the cerebrospinal fluid pressure, as a key factor to help explain the role of IOP. He shows a series of experiments demonstrating how translaminar pressure gradient affects neural function, blood vessels, and connective tissue in glaucoma.

Transcleral Cyclophotocoagulation: from the classics to the moderns

Transcleral cyclophotocoagulation
Dr. Paul Chew spoke on Micropulse Transscleral Cyclophototherapy. He talked about how Micropulse (Transcleral) Pars Plana Phototherapy (MP3) results in increased uveoscleral outflow in a nondestructive, non-thermal manner. The IOP reduction with the MP3 is similar to conventional Transscleral cyclophotocoagulation(TSCPC), but is more consistent and more predictable, without the risk of hypotony.

Training glaucoma surgeons in West Africa

Training eye case professionals
Dr. Catherine Green discussed how to train eye care providers, highlighting the fact that money alone will not solve the problem, and that attention should be addressed to how and not only to what must be learned, and concluded with a description of the “Pacific Islands project”.

Track my visual field in lockdown…

Trabeculotomy: quadrant approach verse 360 degree surgery
(1) Circumferential (360 degree) trabeculotomy might be more effective in primary and secondary congenital glaucoma than a quadrant approach with metal probes as a primary procedure.
(2) A two level scleral dissection seems to be safer for finding Schlemm’s canal in circumferential trabeculotomy
(3) Severity of congenital glaucoma might be crucial for surgical outcome and prognosis
(3) The role of trabeculotomy, trabeculectomy or tubes in far advanced, secondary or recurrent congenital glaucoma is still not established
From the Education Committee
Dr. Grehn discussed the challenges of trabeculotomy in pediatric glaucoma. He also discussed in detail the steps of conventional trabeculotomy and also elaborated on his way of doing the procedure which included a two level approach to Schlemm’s canal. He also spoke on the outcomes of conventional trabeculotomy. He later elaborated the procedure of 360 degree trabeculotomy and compared the success of this procedure against that of conventional trabeculotomy.

Trabeculotomy
trabectome can be performed in a broad spectrum of disease severity and for any age with robust outcomes.
From the Education Committee
Dr. Sameh Mosaed talked about ab interno trabeculotomy using the Trabectome system. She highlighted the fact that this MIGS procedure can be performed anywhere along the spectrum of the disease and is appropriate for target IOP in mid teens. She talked about the outcome analysis of the available global Trabectome experience and the outcome data from the literature. Broadly, patients undergoing Trabectome had about 30% IOP reduction and a 60% reduction in glaucoma medications.

Trabeculoplasty
Dr. Mark Latina gave an update on how to best use Selective Laser Trabeculoplasty (SLT) in clinical practice. He talked about choosing SLT early in the course of therapy, as 360 degrees of SLT gives approximately 30% IOP reduction (similar to prostaglandins) with 100% compliance, 85-90% success rate and negligible adverse effects. The efficacy of SLT drops to half if used later as a second line of therapy. He highlighted the value of SLT to the MIGS canal procedures. He introduced the new rotating SLT lens, the Latina indexing goniolens. He also reported a new technique adopted by Dr Michael Belkin, using transscleral SLT without a goniolens, resulting in about 20% IOP reduction.

Trabeculectomy with releasable / adjustable sutures

Trabeculectomy with mitomycin C alone or coupled with intracamerular bevacizumab? A two year comparative study

Trabeculectomy with adjustable/ releasable sutures

Trabeculectomy in high Myopia

Trabeculectomy in children
Dr Khaw elaborated each step of trabeculectomy in detail and highlighted the precautions required in each step to prevent the possible early and late complications. He discussed the Moorfields safer surgery system and how this technique has reduced the incidence of post-trabeculectomy complications in children.

Trabeculectomy and combined surgery

Trabeculectomy and combination with trabeculotomy

Trabecular MIGS Pro-active treatment evidences: who (really) needs it?

Trabecular MIGS are cost effective in real world:Yes

Trabecular MIGS are cost effective in real world:No

Trabecular Meshwork Scarring & ROCK inhibitors

Trabecular meshwork biomechanics
Dr. Darryl Overby next discussed the biomechanics of the trabecular meshwork, presenting a hypothesis of outflow homeostasis involving an active mechanism regulating trabecular meshwork resistance, involving concepts such as trabecular meshwork stiffnes, shearing forces, nitrous oxide and feedback mechanisms.

Trabecular cutting procedures (KDB, BANG, GATT, microhook)

Trabecular bypass – Stenting is better than cutting

Trabecular bypass – Stenting is better than Cutting

Trabecular bypass – Cutting is better than Stenting

Trabecular bypass implants

Trabecular bypass devices: iStent & Hydrus

Trabecular bypass – KDB vs Trabectome

Trabecular bypass – GATT vs viscodilatation

Trabectome and Preserflo after failed canaloplasty

Trabectome
safe and effective MIGS, with longest track record of data of all minimally invasive trabecular bypass procedures

Trab plus – ideal modified Trabeculectomy
Glaucoma surgery has been a paradigm shift. The conventional surgery Trabeculectomy and Tube surgery is being replaced by MIGS and MIBS. This modified trabeculectomy – Trab Plus produces better control of IOP in the advanced and refractory Glaucoma
Dr. Md. Nazrul Islam Bangladesh Eye Hospital & Institute

Trab and trab: Tips and Tricks

Topics on Exfoliation Glaucoma

Topical Glaucoma Treatment: the good and the bad

Too low for Comfort

Too long – too short
Cecilia Fenerty elaborated on the reasons why the intraocular portion of the tube could be too short or too long including surgical technique. She highlighted the importance of good surgical technique and the need to fix the tube adequately to the scleral bed. She described very useful techniques for tube extension using a 22 G IV canula and lacrimal tubing.

Tonometry Tips: Perfecting IOP Assessment
This content is only accessible to WGC-2019 participants
Login

TOMEY – Imaging the anterior segment with CASIA2 OCT
Advanced imaging with CASIA2
Enable to obtain wide, deep and clear images of anterior segment
Easy to handle and gentle for patients with non-contact procedure
Useful for angle closure diagnosis
Useful for diagnosis with compromised cornea
Useful for surgical treatment of glaucoma
- Applications of CASIA2 OCT for clinical diagnosis
Makoto Aihara - Advances in anterior chamber angle measurements with CASIA2 OCT
Christopher Leung - Measurement of the anterior chamber angle with CASIA2 OCT
Shan Lin - Sharing research data in glaucoma by using CASIA and CASIA2 OCT
Xiulan Zhang

To tunnel or not to tunnel
This content is restricted and only accessible to WGC-2019 participants
Login

To Patch or Not to Patch: Options for Covering the Tube

Tissue engineering for the anterior segment

Tips to master the art of intra-operative gonioscopy: a necessary skill for ab-interno MIGS
We shall demonstrate the tips for optimal angle visualization intra-operatively, addressing changes in microscope & patient position, surgeon’s ergonomics, techniques, and challenges to acquire an un-interrupted enface view of the angle during MIGS
Professor Graham A Lee, University of Queensland, Australia

Tips for MIGS

Tips for intraoperative gonioscopy and how to perform goniosynechiolysis | Kazuhiko Mori
Increasingly, glaucoma specialists require expertise in surgical gonioscopy, as lots of MIGS procedures with ab interno approaches utilize a surgical goniolens.
Goniosynechialysis (GSL), which physically separates peripheral anterior synechiae from trabecular meshwork, also utilizes surgical goniolens. There are two types of surgical goniolens; direct type and double mirror type. Direct gonioprisms which have been widely used require a tilt of the patients’ head and/or microscope, while double mirror goniolens allows the surgeons to perform gonio surgery without tilting the head or microscope.
In this video, tips and pitfalls of using surgical goniolens and performing GSL are presented. The keys for success are keeping the visualization optimized and never losing the view of the mirror or prism. In cases of phaco combined with angle/gonio surgery, phaco before or after depends on the surgeon’s choice, however, from the standpoint of optimizing visualization, performing the angle/gonio surgery in advance is recommended unless there are any problems.

Tips and Pearls of Trabeculectomy

Three-year results of a Supraciliary Drainage Device in Patients with Open Angle Glaucoma

This video is exclusively available to WGC-2025 participants
Welcome! We’re glad you’re here.
Log in below with your WGA#One account if you registered for WGC-2025
Forgot password? | Need help?
The World Glaucoma Association in a nutshell
Always wanted to know what the WGA is all about? Find out in less than two minutes.
At the World Glaucoma Congress 2019 in Melbourne Australia, host Josh Szeps sat down with Keith Martin (President WGA 2017-2019), Anne Brooks (President ANZGS), Shan Lin (Executive Vice President WGA) and Kaweh Mansouri (Associate Executive Vice President WGA) to talk about the World Glaucoma Association.

The World Glaucoma Association during the COVID-19 Pandemic
The WGA’s Commitment to Glaucoma Care in Africa

The use of transscleral cyclophotomodulation in patients with glaucoma

The Translaminar Pressure Difference: Key to Glaucoma?
The orbital cerebrospinal fluid pressure as the counter-pressure against the intraocular pressure across the lamina crirbosa may be further discussed of having an influence on glaucomatous optic neuropathy

The structure-function relationship in glaucoma

The science and evolution of xen

The Role of Pupillary Block

The Role of Phacoemulsification in the Management of Primary Angle Closure Glaucoma

The role of OCT-A in clinical glaucoma
OCTA parameters have comparable diagnostic accuracy to OCT RNFL thickness. OCTA may be able to detect glaucoma progression earlier than OCT. Older age, male sex, longer diabetes duration, and longer axial length are associated with reduced peripapillary vessel density. Qualitative identification of wedge defects on OCTA can be helpful in detection of early glaucoma.
From the Education Committee
Dr. Grace Richter next discussed the role of OCT-A in clinical practice, analyzing data and presenting specific cases, correlating and distinguishing diagnostic abilities and differences between OCT and OCT-A. Systemic and non-glaucomatous associations, such as diabetes and myopic are further discussed. Last, individual patient data is presented, highlighting the value of the OCT-A scan.

The Role of Microvasculature in the Pathophysiology of Glaucoma: Evidence from OCT Angiography
Mirroring Prof Kim’s view of the uncertainty in the sequences of events of microvascular changes in glaucoma pathogenesis, Prof Zangwill suggested that in some individuals, vascular changes are the primary event, whereas in others, mechanical damage may be the primary event. She then described the relationship between vascular and mechanical factors in the pathophysiology of glaucoma, which was assessed by evaluating vessel density in glaucomatous eyes with and without lamina cribrosa defect. She ended her talk by suggesting the need for longitudinal OCTA studies that would provide valuable information that may help improve our understanding of the pathophysiology of glaucoma.

The Role of Laser Surgery in Africa
Selective laser trabeculoplasty has the potential to reduce vision loss and blindness from glaucoma in sub-Saharan Africa.

The role of autoimmunity and glaucoma therapy
Autoimmunity plays a critical role in glaucoma.
Patients may present with different autoantibodies (down-or upregulated)
Research may lead to personalized treatment in glaucoma

The role of anterior segment imaging in glaucoma management

The role of AI in clinical practice
1. AI will sharply improve glaucoma diagnosis.
2. Diagnostic algorithms based on multi-modular imaging data may have better performance than those based on single- modular data.

The risk is not same for all: Understanding differences in genetic predisposition across race

The retinal nerve fiber layer in myopia – implications for glaucoma
There are significant differences in the RNFL measurements in myopic subjects without glaucoma. The RNFLT variations including thinning in the different quadrants may occur, making it difficult to differentiate from glaucomatous thinning. The RNFL thickness is not only influenced by axial length, but also by the presence or absence of gamma zone, by the vascular origins from the optic disc and asymmetric elongation of the eye. In eyes suspected to having glaucoma, follow up of the RNFL may be important.
From the Education Committee
Dr. Vinay Nangia spoke on Retinal nerve fiber layer thickness in myopia in relation to glaucoma. He highlighted that there were several parameters besides axial length, which influenced the RNFL thickness in myopes. These included the size of optic disc, disc diameter, presence of gamma zone, centration of RNFL circle, pattern of vascular origins from the optic disc and possible asymmetric changes in the axial length of the eye.

The results of treatment of neovascular glaucoma with intravitreal injections

The results of glaucoma surgeries with silicone tube implants in neovascular glaucoma
The Relation Between Trans-Lamina Cribrosa Pressure Difference and Primary Open Angle Glaucoma Among Newly Discovered Sudanese Patients, at Makkah Eye Complex-Khartoum, Sudan in 2018-2019

The published experience of collaborative care
Reduction in follow up delays
• Reducing the risk of vision loss related to glaucoma
• Education – discussing compliance
• Detecting other pathology
• Consultant clinic slots freed
From the Education Committee
Dr. Verona Botha shared her experience on a collaborative care glaucoma clinic in New Zealand. Despite the increase in patients and visits over 5 years, in a scenario of collaborative care among ophthalmologists and optometrists, there was a significant reduction in uncontrolled IOP patients, as well as progression rate. A reduction in follow up delays and in waiting times was demonstrated. Another benefit was the detection of other pathologies.

The promise of RGC transplantation
Increasing success in animal model, potential for human therapy remains uncertain

The problem of Glaucoma care in Ukraine during wartime

The Problem & Magnitude of Blindness from Glaucoma in Sub-Saharan Africa

The prevalence of OCT artifacts in high myopia and its influence on glaucoma diagnosis

The physical and chemical properties of antiglaucomatous eye drops

The pathology of exfoliation syndrome-a clinician’s perspective
Deepak Edward, MD, ended the session talking about the pathology of exfoliation syndrome from a clinician’s perspective. He described the clinical feature of XFS and the importance of looking for them during a complete ophthalmic examination. The focused on the clinical-pathological correlations between slit-lamp findings (including reasons why XFG eyes are more challenging during cataract extraction) and histological characteristics.

The paradox of PACG – how some eyes can tolerate appositional closure for years while some eyes get blinding disease (Epi / Genetics – Basic Science)

The overfiltering bleb
In overfiltering blebs this method is straight forward, minimally invasive and easy to perform. However, visibility of the scleral flap is mandatory for correct positioning of the sutures.

The Outcome Measures
Glaucoma definition, diagnostic criterion and subsequent quality of glaucoma care must be consistent and meaningful for multiple levels of careproviders . A list of outcome measures is needed that can be used to evaluate if the treatment for glaucoma does any good to the patients. In addition to the patient, societal and clinician domains, outcome measures can be analysed as direct and intermediate outcome measures.

The numerous ways in which glaucoma affects our patients
In moderate to advanced disease, glaucoma can affect the visual function of an individual – seeing at night, walking on uneven surface or in the dark, adjusting to changes of lighting, which may affect their reading, gait and influence falls risk and driving. Glaucoma can also influence psychological morbidity (anxiety and depression) and treatment for glaucoma can influence ocular surface disease. Concern for future generations, cost and imposition of regular monitoring and treatments are also associated with glaucoma’s psychosocial impact

The Novel 4D Cost Effective Holographic Glaucoma AI Metaverse with Augmented Reality

The Next Generation of Trabecular Micro-Bypass Stents

The New EGS Guidelines

The new EGS Fellowship

The many issues of glaucoma medication adherence

The Magnitude and Burden of Glaucoma in Africa

The Legacy: Preparing for the Future
This film shows how a medical institution trains glaucoma specialists to bring advanced skills back to their countries. Through collaboration strategies, fellows become leaders in eye care, ready to improve glaucoma management globally.
WILLIAM MCCOLLUM – Producer – Hospital Dr. Elías Santana CCSM LLOYD DIAZ – Co-Producer – Hospital Dr. Elías Santana CCSM JOSEPH HUNTER – Editor – Hospital Dr. Elías Santana CCSM Participants: JUAN BATLLE, MARGARITA ARBAJE, CAROLINA RODRIGUEZ, RODRIGO RIVERA AND NAHOM AYALEW

The leaking bleb

The infected bleb
Prevention measures and early diagnosis are key in management of infection after trabeculectomy

The importance of combining structure and function

The Impact of Ageing upon the Optic Nerve Head
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login

The ICO-WGA Fellowship Program
The ICO-World Glaucoma Association Three Month Fellowship Program is organized to help promising young ophthalmologists from developing countries improve their practical skills and broaden their perspectives of ophthalmology and glaucoma.
At the World Glaucoma Congress 2019 in Melbourne Australia, Neeru Gupta (President-Elect WGA) presented the 2019 Award to 5 Fellows from sub-Saharan Africa. Paul Healey (Treasurer WGA) presented the future of the program.

The gold standard: trabeculectomy
Trabeculectomy is a high yield , high risk and high maintenance surgery and there is an unmet need to improve efficacy and safety outcomes. The following modifications can help to achieve this :
-Use of pre-operative steroids to reduce conjunctival inflammation
– Avoiding superior rectus traction suture
– Using Anterior chamber maintainer
– Not exceeding 0.2mg/ml of MMC for 3 minutes
– Creating an intrascleral lake with limited deep sclrectomy
– Using releasable sutures
– Surgical repair of bleb leaks

The glaucoma triumvirate- IOP, CNS and venous pressure at the optic nerve head

The glaucoma triumvirate- IOP, CNS and venous pressure at the optic nerve head

The girl who was afraid of darkness

The Gillies Lecture: Of Glaucoma, Prevention of Blindness & the Reverend: A personal Khichdi
The effect of dynamic iris changes and its association with PACS and PACG has been well established in cases with pupillary block. Case detection in the clinic strategy is a better tool for the early detection of PACD as the tools available have high specificity and moderate sensitivity. Cataract extraction lowers the IOP by 2-3 mm in most eyes and works best in eyes with PACG eyes showing slightly better response than POAG.
From the Education Committee
Dr. Ravi Thomas describes the prevalence of angle closure and open angle glaucoma in India, as well the rate of conversion from primary angle closure suspect and primary angle closure to angle closure glaucoma. He discussed the impact of cataract extraction on intraocular pressure as well as factors that may predict greater pressure lowering. In addition, he discusses the effect of Vitamin A deficiency and malnutrition on rates of blindness and visual impairment.

The Future of the Clinical Examination

The Filipino Adaptation of the Glaucoma Medication Adherence Self Efficacy Questionnaire

The evolving role of fixed combination therapy in glaucoma

The Eroded Tube

The epidemiology of glaucoma in Asia

The encapsulated bleb
Prevention and early recognition of bleb encapsulation is essential to increase chances of trabeculectomy success. Timely adjustment of topical steroids, subconjunctival anti-VEGF, 5FU or MMC and Needling can help prevent bleb encapsulation.
For established encapsulation medical treatment with steroids and aqueous suppressants are often successful, and appear to be at least as successful as needling.

The Effect of Converting from SITA Standard to SITA Faster on Visual Field Performance

The effect of cataract surgery on IOP

The dysesthetic bleb
Management should focus on IOP control and patient discomfort

The dual role of LOXL1 in exfoliation syndrome/glaucoma
Pseudoexfoliation syndrome is a complex disease, which is crucially influenced by coding and non-coding variants in the LOXL1 gene impacting on both LOXL1 function and expression. In particular, dysregulated expression of LOXL1 plays a key role in pathogenesis and glaucoma development by contributing both to the formation of fibrillar aggregates and to elastotic-degenerative connective tissue alterations. Environmental and dietary factors as well as epigenetic alterations likely modify disease risk in genetically predisposed individuals.
From the Education Committee
Ursula Schlötzer explains the role of LOXL1 gene in formation of elastic fibers and how dysregulation of this gene affects the eye. In this presentation find out about the formation of PEX material and the disease progresses from preclinical stages to clinically apparent manifestations and finally to glaucoma.

The difficult and unusual

The corruption of evidence based medicine

The Changing Landscape of Glaucoma Research: Who is doing it? And where is it being done?

The change of optic nerve head during axial elongation and its relation with glaucoma
The association of axial elongation with Optic Nerve Head and peripapillary tissue changes may facilitate understanding of the relationship between myopia and glaucoma. Because the central retinal vascular trunk is embedded in the lamina cribrosa(LC), its dragging indicates nasal shifting , which could explain the development of focal lamina cribrosa defects and the vulnerability of myopic eyes to glaucomatous optic neuropathy.

The challenges of Pseudoexfoliative glaucoma
‘- Pseudoexfoliative glaucoma is an aggressive subtype of OAG that needs special attention
– Many advantages to performing cataract surgery early in PEXG patients
– If cataract surgery is performed after filtration surgery, extra pre- and postoperative care is needed
– PEX is an ocular manifestation of a systemic disease but no need for additional investigation solely based on presence of PEX
From the Education Committee
Challenges in pseudoexfoliative (PXF) glaucoma were discussed by Gauti Johannesson. Dr. Johannesson reviewed the aggressive course which often accompanies PXF glaucoma, as demonstrated by the Early Manifest Glaucoma Trial (EMGT). Challenges in managing PXF include lens related issues (i.e. lens/IOL dislocation) and more complications at the time of cataract surgery. Using various patient examples, he discusses both the pros of early cataract surgery (i.e. enjoying the IOP-lowering effect), and also the cons of early cataract surgery (more time for IOL displacement later), suggesting that early cataract surgery is generally a good idea. He also discusses whether additional challenges are present which guide how the patient should be managed medically by their primary doctor, suggesting that no additional health checks or screening exams are required.

The central visual field in glaucoma

The association between blood pressure and open angle glaucoma in a U.S. nationwide retrospective electronic health records cohort study

The 5th APTOS Symposium
The 5th Asia Pacific Tele-Ophthalmology Society (APTOS) Symposium
Featuring top-notch speakers from Korea and around the world, APTOS 2020 will showcase clinical applications of artificial intelligence in telemedicine and the role tele-ophthalmology plays in reaching the unreached and in difficult circumstances in which the physicians and the patients are miles apart. We have not imagined we can be working from home for so long that people start to talk about having a virtual office. By the same token, while we can’t imagine having a virtual clinic right now, we can be sure that technology will keep advancing and one day, it will become a new normal for all of us.
We look forward to seeing you online.
For more information please visit the website here
The 5th Congress of the Serbian Glaucoma Society
Join the 5th congress of the Serbian Glaucoma Society which will take place between 12-15 May 2022, in Serbia.
For more information visit their website: http://www.uglaukomatologa.rs//.
The 41st Asia-Pacific Academy of Ophthalmology Congress
The 41st Asia-Pacific Academy of Ophthalmology Congress in conjunction with The 37th Annual Scientific Meeting Hong Kong Ophthalmological Symposium will be held in Hong Kong from February 5 – 8, 2026 at the Hong Kong Convention and Exhibition Centre.
More information about APAO 2026 can be found here.
The 38th Asia-Pacific Academy of Ophthalmology Congress
Join the 38th APAO Congress! The congress will take place from February 23-26, 2023, in Kuala Lumpur, Malaysia. Visit WGA booth at APAO Congress: #7075
For more information visit their website: https://apaophth.org/
The 36th Meeting of Japan Glaucoma Society
The 36th Annual Meeting of the Japan Glaucoma Society will be held at Kobe Portopia Hotel on September 12 (Fri.) ~ 14 (Sun.), 2025. This will be the first time in 19 years that the Society has been held in Kobe, since the 17th Conference, which was held in 2006 by President Akira Neki. Dr. Kurimoto of Kobe Eye Center Hospital served as the president of the university, and Dr. Kiyomi Furukawa, president of the Hyogo Ophthalmologists Association, served as the vice president.
Find out more about this event here.
The 33rd Meeting of the Japan Glaucoma Society
Join the Japanese Glaucoma Society for their 33rd Annual Meeting.
For more information visit the JGS website here .
The 32nd Meeting of the Japan Glaucoma Society
The 32nd Meeting of the Japan Glaucoma Society (JGS)
Join the Japanese Glaucoma Society for their 32nd Annual Meeting.
For more information visit the JGS website here .
The 26th Congress of the Chinese Ophthalmological Society
The 26th Congress of the Chinese Ophthalmological Society
Join the Chinese Ophthalmological Society for their 26th National Congress, taking place from August 25-29, 2021.
For more information visit: https://ccos2021.sciconf.cn/cn/web/index/10899_ .

The 22nd Annual Meeting of the Egyptian Society for the Glaucomas
Join the 22nd Annual Meeting of the Egyptian Society for the Glaucomas (ESG2022) which will take place in Cairo from November 24-25, 2022.
For more information visit their website: https://esg2022.org/
The 2021 EVER Festival
The 2021 EVER Festival
Join the European Association for Vision and Eye Research for the 2021 EVER Festival, taking place from September 27 – October 2, 2021.
For more information visit: https://www.everassociation.org/

The 16th Congreso de la Sociedad Española de Glaucoma
Join the 16th annual congress of the Spanish Glaucoma Society which will take place between 10-12 March 2022, in Mallorca, Spain.
For more information visit their website: https://www.sociedadglaucoma.com/xvi-congreso-de-la-sociedad-espanola-de-glaucoma/.
The 125th Annual Meeting of the Japanese Ophthalmological Society
The 125th Annual Meeting of the Japanese Ophthalmological Society
Join the Japanese Ophthalmological Society for their 125th Annual Meeting. This meeting will be held as a hybrid meeting, meaning there will be a physical meeting when government regulations allow this, as well as the opportunity to watch the content online, on-demand.
For more information visit the JOS congress website here .
The 124th Annual Meeting of the Japanese Ophthalmological Society
The 124th Annual Meeting of the Japanese Ophthalmological Society
The 124th Annual Meeting of the Japanese Ophthalmological Society in 2020 will be organized by the Department of Ophthalmology of the Tokyo Medical University. The theme of the Annual Meeting is “2020: Learn from History, Connect to the Future”. In ophthalmology, twenty-twenty (20-20) is a number or an expression that represents “visual acuity 1.0” or “good vision”. In addition, the year 2020 is a memorable year because the Olympic and Paralympic Games will take place in Tokyo, 56 years after the city first hosted the Olympic Games in 1964. The environment surrounding ophthalmology has changed remarkably during the last half-century, and further developments are expected in the future. To commemorate the special year of 2020, we wish to spotlight on the achievements of our predecessors and to confirm their wisdom once again, in order to connect to future prospects. That is the reason for choosing the theme of this Annual Meeting.

The 11th ICGS
The 11th International Congress on Glaucoma Surgery (ICGS)
Join the 11th ICGS which will take place in person, between 21-23 April 2022, in Geneva, Switzerland.
For more information, and registration: https://icgscongress.org/.
Thank You for Purchase
Thanks for purchasing the course, your order will be processed shortly.
Testing strategies for detecting glaucoma
Imaging of the retinal nerve fibre layer, optic nerve head and macula can aid glaucoma detection but should only be used in conjunction with other information including tests of visual function.
From the Education Committee
Big data is extremely large data sets that may be analyzed computationally to reveal patterns, trends, and associations that relate especially to human behavior and interactions. Do we have the big data about glaucoma?
Detecting glaucoma requires a thorough analysis along with a relevant examination of risk factors and changes in structure and function. Dr. Tatham lectures about the specificity and sensitivity as well as the strengths and limitations of these tests. Access to modern technology in low income countries is challenging but the necessity for diagnosis, documentation and follow-up supersedes these challenges because the rate of blindness and advanced glaucoma are becoming more frequent. Dr. Philippin shows how to use smartphone cameras, low cost ophthalmoscopes as well as how to conduct visual field tests with a laptop in underdeveloped areas.
Open angle glaucoma has a significant genetic component with a relative risk of over 9 in first-degree relatives of affected individuals when compared to relatives of unaffected people. Genome-wide association studies (GWAS) have now successfully identified important genetic variants associated with many human traits and diseases. Dr. Hewitt introduces us to this innovative and groundbreaking topic. After, Dr. Craig addresses interactions between genes and their environments with valuable examples about the upregulation of the myocilin gene with steroids and the increased expression of LOXL1 under UV irradiation in Pseudoexfoliation.
What information enables an analysis of half million of the visual field? David Crabb provides data of VF progression, the initial presentation stage of glaucoma, and the right frequency of testing that may surprise you as well as save costs in the health care system.

Testing of the more central visual field

Testing – when to do more, and when to do less

TEST EVENT RSVP
The World Glaucoma Association is launching a new series of webinars focused on surgical challenges that glaucoma specialists are likely to face: WGA Surgical Grand Rounds. Each 1-hour webinar will feature two scenarios of surgical challenges or complications. After each presentation, the speaker will join an expert panel for a brief discussion and answer questions related to the presentation. Get ready for state-of-the-art surgery videos and discussions from the world’s most skillful glaucoma surgeons!
Join us at the first-ever edition of the WGA Surgical Grand Rounds on Thursday, January 27, 2022, in 3 easy steps:
- Enter your details below
- Confirm your registration by clicking on the link in the email
- Join one of the two broadcasts!
Register here
Test Broadcast v2
Join the conversation
Joining the live chat is the best way to get involved during the WGA Surgical Grands Rounds webinar: connecting with other attendees and asking questions. Learn how to join the live chat here.
Join the conversation
Joining the live chat is the best way to get involved during the WGA Surgical Grands Rounds webinar: connecting with other attendees and asking questions. Learn how to join the live chat here.
Terms and Conditions
Privacy Policy
We respect your privacy
Generally, World Glaucoma Association uses data collected to improve its own web content; to respond to visitors’ interests, needs and preferences; and to develop new products and services. Any personal information you provide to us including and similar to your name, address, telephone number and email address will not be released, sold, or rented to any entities or individuals outside of our organisation except as noted below.
What personal information we collect
The services we provide require us to collect personal data about our users, which may include the individual’s name, email address, telephone number, and employer, date of birth and professional interest areas.
How we collect information
World Glaucoma Association may collect personal information from you when you:
- Register to attend an event
- Purchase a publication
- Sign up for a web account
- Become a member
- Submit details on our websites
You can always choose not to provide your personal details to World Glaucoma Association, but it may mean we are unable to provide you with the service. The websites of the World Glaucoma Association include: www.worldglaucoma.org, www.worldglaucomacongress.org, www.worldglaucomaweek.org and www.e-igr.com.
To gain access to members-only resources and personalization features on worldglaucoma.org, members and other users are asked to register and provide specific information. This information is submitted voluntarily. World Glaucoma Association asks users to provide their name, organisation name, business phone, and e-mail. Similar information may be submitted to World Glaucoma Association through membership applications, conference or seminar registration, publication orders and subscriptions.
Additionally, for some emails sent in HTML format by World Glaucoma Association to its members through electronic newsletters, we will collect specific information regarding what the recipient does with that email. For those emails, World Glaucoma Association will monitor whether a recipient subsequently clicks through to links provided in the message. Other information collected through this tracking feature includes: email address of a user, the date and time of the user’s “click,” a message number, name of the list from which the message was sent, tracking URL number and destination page. World Glaucoma Association only uses this information to enhance its products and distribution of those products to its members. This information is not sold or distributed in any other manner.
How information can be accessed and corrected
You may access your personal information at any time by logging into your personal account on our website at worldglaucoma.org. To ensure your information is accurate, we encourage you to login to your account and review your personal information. You can update any incorrect information via your online account or alternatively by contacting us at info@worldglaucoma.org or on +31 20 570 96 00. Any correction requests received will be processed within 5 working days except in extraordinary circumstances.
How to complain
Should you have any complaints relating to our collection or use of your personal information you should contact us at info@worldglaucoma.org. We request that complaints be lodged via email for audit trail purposes and to ensure a prompt and transparent resolution process.
Where your information is stored
All of our data, including personal and non-personal information is stored on our servers. Our primary database is hosted on a server in Amsterdam, The Netherlands, and this is where the majority of your personal information will be stored. As we utilize cloud technology and our website providers are located in The Netherlands, your personal information may also be stored on a server in The Netherlands.
By providing your personal information to World Glaucoma Association, you consent to World Glaucoma Association storing your personal information on our servers in The Netherlands.
Our service providers
We may share your personal information with companies that perform services on our behalf, for example, companies that help process credit card payments, deliver our congresses and events, and provide services on behalf of World Glaucoma Association. This includes, but is not limited to, THGF, MCI, Kugler Publications, Conference Compass and Fundación OFEC. Our service providers are required by contract to protect the confidentiality of the personal information we share with them and to use it only to provide specific services on our behalf.
Disclosures to third parties
World Glaucoma Association also makes member contact information available through the World Glaucoma Association Membership Directory to other members using its website and to those who register for its congresses.
On occasion, World Glaucoma Association may also provide limited data to third parties that offer products and services. These limited data include companies and business addresses, but do not include names, job titles, business phone numbers, business fax numbers or email addresses. Users may request World Glaucoma Association refrain from disclosing the data it collects to third parties on the membership application form, congress registration form or any other form on which they are providing information; an opt-out box will appear on each form on which a user provides information.
Alternatively, users may contact World Glaucoma Association at info@worldglaucoma.org to express their preferences that they do not wish to have the information shared.
Business transfers
Your personal information may be transferred to another entity (either an affiliated entity or an unrelated third party) in connection with a merger, reorganization, dissolution or similar corporate event. If such a transfer were ever to occur, the acquiring entity’s use of your personal information will still be subject to this Privacy Policy.
Government and legal disclosures
We may disclose the personal information we collect through this site, when we, in good faith, believe disclosure is appropriate to comply with the law (or a court order or subpoena); to prevent or investigate a possible crime, such as fraud or identity theft; to enforce our Terms and Conditions or other agreements that govern your use of this site; or to protect the rights, property or safety of our company, our users, or others.
Cross-border disclosures
Service providers and other entities with whom we may disclose your personal information may be located outside of The Netherlands.
While your personal information will be disclosed through the central World Glaucoma Association Database, internal policies and procedures restrict foreign entities from using, disclosing, extracting or editing your personal information.
Service providers located outside The Netherlands are bound by confidentiality agreements and are not permitted to use, disclose, extract or edit your personal information unless doing so in accordance with World Glaucoma Association related activities. We currently have service providers in The Netherlands. These service providers are contracted to provide database management services to World Glaucoma Association.
External sites
We are not responsible for the content of external internet sites. You are advised to read the privacy policy of external sites before disclosing any personal information.
Cookies
A “cookie” is a small data text file that is placed in your browser and allows us to recognize you each time you visit this site (personalization, etc). Cookies themselves do not contain any personal information, and we do not use cookies to collect personal information. Cookies may also be used by 3rd party content providers such as newsfeeds.
Remember the risks whenever you use the internet
While we do our best to protect your personal information, we cannot guarantee the security of any information that you transmit to us and you are solely responsible for maintaining the secrecy of any passwords or other account information. In addition, other internet sites or services that may be accessible through our site have separate data and privacy practices independent of us, and therefore we disclaim any responsibility or liability for their policies or actions. Please contact those vendors and others directly if you have any questions about their privacy policies.
Code of Conduct
Community Rules & Etiquette
Thank you for being part of our community. To ensure the best possible experience for all members, we have established some basic guidelines for participation.
By joining and using this community, you agree that you have read and will follow these rules and guidelines. You also agree to reserve discussions and shared files and content to that best suited to the medium. This is a great medium with which to solicit the advice of your peers, benefit from their experience, and participate in an ongoing conversation. Please take a moment to acquaint yourself with these important guidelines. If you have questions, contact the World Glaucoma Association Executive Office. In order to preserve a climate that encourages both civil and fruitful dialogue, we reserve the right to suspend or terminate membership in this community for anyone who violate these rules.
The rules
- Do not challenge or attack others. The discussions and comments are meant to stimulate conversation not to create contention. Let others have their say, just as you may.
- Do not post commercial or advertising messages on any discussion list, resource library entry, or other area where others might see it. Contact people directly with product and service information if you believe it would help them.
- Use caution when discussing products. Information posted on the lists and in the libraries is available for all community members to see, and comments are subject to libel, slander, and antitrust laws.
- All defamatory, abusive, profane, threatening, offensive, or illegal materials are strictly prohibited. Do not post anything that you would not want the world to see or that you would not want anyone to know came from you.
- Please note carefully all items listed in the disclaimer and legal rules below, particularly regarding the copyright ownership of information posted.
- Remember that other participants have the right to reproduce postings to this site unless you specify otherwise.
- Post your message or documents only to the most appropriate lists or libraries. Do not spam several lists or libraries with the same message.
- All messages must add to the body of knowledge. We reserve the right to reject any message for any reason.
Discussion group etiquette
- Include a signature tag on all messages. Include your name, affiliation, location.
- State concisely and clearly the topic of your comments in the subject line. This allows members to respond more appropriately to your posting and makes it easier for members to search the archives by subject.
- Include only the relevant portions of the original message in your reply. Delete any header information, and put your response before the original posting.
- Only send a message to the entire list when it contains information that everyone can benefit from.
- Send messages such as “thanks for the information” or “me too” to individuals-not to the entire list.
- Do not send administrative messages, such as remove me from the list. Instead, use the web interface to change your settings or to remove yourself from a list. If you are changing email addresses, you do not need to remove yourself from the list and rejoin under your new email address. Simply change your personal settings.
- Warn other list subscribers of lengthy messages either in the subject line or at the beginning of the message body with a line that says “Long Message.”
The legal matters
This site is provided as a service for the members of World Glaucoma Association. World Glaucoma Association is not responsible for the opinions and information posted on this site by others. We disclaim all warranties with regard to information posted on this site, whether posted by World Glaucoma Association or any third party; this disclaimer includes all implied warranties of merchantability and fitness. In no event shall World Glaucoma Association be liable for any special, indirect, or consequential damages or any damages whatsoever resulting from loss of use, data, or profits, arising out of or in connection with the use or performance of any information posted on this site.
Do not post any defamatory, abusive, profane, threatening, offensive, or illegal materials. Do not post any information or other material protected by copyright without the permission of the copyright owner. By posting material, the posting party warrants and represents that he or she owns the copyright with respect to such material or has received permission from the copyright owner. In addition, the posting party grants World Glaucoma Association and users of this site the nonexclusive right and license to display, copy, publish, distribute, transmit, print, and use such information or other material.
Messages should not be posted if they encourage or facilitate members to arrive at any agreement that either expressly or impliedly leads to price fixing, a boycott of another’s business, or other conduct intended to illegally restrict free trade. Messages that encourage or facilitate an agreement about the following subjects are inappropriate: prices, discounts, or terms or conditions of sale; salaries; profits, profit margins, or cost data; market shares, sales territories, or markets; allocation of customers or territories; or selection, rejection, or termination of customers or suppliers.
World Glaucoma Association does not actively monitor the site for inappropriate postings and does not on its own undertake editorial control of postings. However, in the event that any inappropriate posting is brought to the attention of World Glaucoma Association we will take all appropriate action. World Glaucoma Association reserves the right to terminate access to any user who does not abide by these guidelines.
Policy for member community violations
The World Glaucoma Association community rules and etiquette should not be seen as all-inclusive, but rather to give our members a general idea of the guidelines one should follow when participating in the online community. In order to preserve a climate that encourages both civil and fruitful dialogue, World Glaucoma Association reserves the right to suspend, remove content, or terminate participation on all lists for members who violate these rules.
Taking action against one of our members, particularly in regard to removing an account, is something we would like to avoid, but realistically may have to happen in order to protect the quality of service we strive to provide to our members. This restriction is not intended to limit in any way the professional networking and educational advantages of the World Glaucoma Association community platform.
When unsure whether content is consistent with these policies, please err on the side of caution and do not post the content in the community platform. If there are any questions on what content is appropriate to post please contact the Operations Manager.
The community rules and etiquette may be revised from time to time and it’s the member’s responsibility to stay abreast of any changes.
Possible disciplinary actions for Rules and Etiquette violations
- An email, private message or phone call is communicated to the member that explains the violation that occurred.
- An email or phone call is communicated to the member who violated the guidelines. The member’s community account may be put into moderation. Member may be placed in a 30-day moderation queue, where messages from his/her account are reviewed by the operations manager before they are posted online.
- An email/private message warning is communicated to the member who violated the guidelines. The member’s community account may be put into moderation. Member may be placed in moderation for three months, where messages from his/her account are reviewed by the operations manager before they are posted online. Member may be subject to removal from communities.
- A formal written letter is sent to the member who violated the guidelines. The member may be removed from participating in some or all communities.
- World Glaucoma Association reserves the right to edit or delete a post. However, World Glaucoma Association generally will not edit or delete posts for members, unless there has been a severe violation of the Rules and Etiquette (as mentioned).
- To clarify or edit a message posted, we recommend the original poster to reply to the existing message. At World Glaucoma Association’s discretion, older messages that may cause confusion or contain outdated information may be archived or deleted.
Appeal process
A member may not appeal his/her moderation reprimand. A member may appeal his/her removal from a community by contacting the operations manager in writing; final decisions will be will be reviewed and decided upon by a panel of peers.
Appeals should include the following pieces of information:
- First name
- Last name
- Email address
- Phone number
- Full disclosure of any previous violations
- Why you feel the community removal should be overturned, include any relevant or supporting evidence.
For any further questions or comments please contact the World Glaucoma Association Executive Office at info@worldglaucoma.org or on +31 20 570 96 00.
Teleglaucoma

Technology to improve communication among allied health professionals

Technology and glaucoma detection in low income populations
High prevalence and incidence of glaucoma as well as glaucoma-related vision impairment, faced by limited human and other resources, are among the characteristics of low-income regions. Technological innovations for structural and functional testing as well as processing of diagnostic information include mobile technology and networks and offer promising prospects.
From the Education Committee
Big data is extremely large data sets that may be analyzed computationally to reveal patterns, trends, and associations that relate especially to human behavior and interactions. Do we have the big data about glaucoma?
Detecting glaucoma requires a thorough analysis along with a relevant examination of risk factors and changes in structure and function. Dr. Tatham lectures about the specificity and sensitivity as well as the strengths and limitations of these tests. Access to modern technology in low income countries is challenging but the necessity for diagnosis, documentation and follow-up supersedes these challenges because the rate of blindness and advanced glaucoma are becoming more frequent. Dr. Philippin shows how to use smartphone cameras, low cost ophthalmoscopes as well as how to conduct visual field tests with a laptop in underdeveloped areas.
Open angle glaucoma has a significant genetic component with a relative risk of over 9 in first-degree relatives of affected individuals when compared to relatives of unaffected people. Genome-wide association studies (GWAS) have now successfully identified important genetic variants associated with many human traits and diseases. Dr. Hewitt introduces us to this innovative and groundbreaking topic. After, Dr. Craig addresses interactions between genes and their environments with valuable examples about the upregulation of the myocilin gene with steroids and the increased expression of LOXL1 under UV irradiation in Pseudoexfoliation.
What information enables an analysis of half million of the visual field? David Crabb provides data of VF progression, the initial presentation stage of glaucoma, and the right frequency of testing that may surprise you as well as save costs in the health care system.

Technique of diluting and giving intravitreal antibiotics | Vijaya Lingam

Teaching residents to deal with low vision
Jack Ciofi talked about integrating vision rehabilitation into ophthalmic training He described his experience at the lighthouse guild and how they had collaborated with this facility to train residents on rehabilitation using both online training and practical exposure. Residents had training programs that spanned all the three years of residency training. In the first year they achieved cognitive milestones, in the second year, technical milestones and in the third year they had practical and constant interactions with patients. He discussed the importance of integrating vision rehabilitation into the resident’s curriculum world- wide.

Targeting the Meshwork- A 21st Century Renaissance
IL-6 trans-signaling suppresses expression of the TGF-β receptors (TGFBR1 and TGFBR2) and thus inhibits fibrogenic changes induced by TGF-B in trabecular meshwork cells.
From the Education Committee
Prof Inoue explains how one success story of targeting the trabecular meshwork for IOP reduction has been achieved with the ROCK inhibitors which are now commonly used for glaucoma treatment. He demonstrated how ROCK inhibitors work by showing time dependent depolymerisation of actin fibres and change of cell shape resulting in wider spaces in the TM and less outflow resistance. He discusses the effect of TGF beta on decreasing outflow facility and caused actin contraction thus being potentially involved in IOP regulation. TGF-β activates Rho-ROCK signalling in TM cells, which is suppressed by ROCK inhibitor. The cross-talk between IL-6 and TGF-β pathway in TM cells and its interaction can in part explain the effect of ROCK inhibitors . He explores the interaction of IL 6 and TGFB receptors 1 and 2 and the interaction between the TGF beta and IL 6 pathways.

Targeting ocular lymphatics in glaucoma

Targeted population screening

Targeted drug delivery as a method of treatment of glaucomatous optic neuropathy

Taking Stock of Minimally Invasive Surgery for Glaucoma: Identity, Evidence and Future

Taking away the driver’s license – when and how?

Take their eyedrops

Tackling the undetected glaucoma polulation

Systemic risk factor modification and non-IOP lowering treatments in the management of NTG
There is no proven treatment alternative to IOP reduction in glaucoma yet. If systemic hypotension seems to play a role in glaucoma progression, coordinate the care with the internist. Consider CCB if patients have evidence of vasospasm. Although several supplements were reported to be beneficial, complementary approaches need to be cautious considering the potential adverse effects.

Systemic medications which may predispose to glaucoma

Systemic Considerations: Looking Beyond the Eye
This content is restricted and only accessible to WGC-2019 participants
Login

Systemic Assessment of Vascular Regulation
Blood pressure (24 hours), vascular dysregulation in relevant vascular beds (retina, retrobulbar circulation) and retinal venous pressure are significant parameters for the evaluation of the ophthalmological vascular status in glaucoma patients. Parameter of interest is also the translaminar pressure gradient, unfortunately we do not have yet clinically routinely applicable methods for this purpose.
From the Education Committee
Prof Konstantin Gugleta pointed out that the autoregulation capacity depended both on Blood pressure (BP;much stronger component) and intraocular pressure (IOP). This capacity can be ascertained by Retinal dynamic vessel analyser. He also talked about the concept of neurovascular coupling and flow mediated dilation.
Retinal Veins have been considered to be passive conductors; but recent studies have shown that they have contractile elements and thus can be modulated both by vasocontraction and vasodilation agents. Although there are no new methods to measure Retinal Venous pressure (RVP), it can be measured by Ophthalmodynamometry. RVP is of significance in Normal Tension Glaucoma and venous occlusion.
He also talked about the Translaminar pressure. Unfortunately, none of the currently available methods to measure it can be used in clinical practice. He suggested that retinal venous pulsations can be a surrogate for translaminar pressure. To ascertain, what is the ‘Pacemaker’ for retinal venous pulsation, he talked about a study that used ECG gated recording of IOP and retinal vein pulsations and found similar pattern in retinal vein diameter and IOP.
He said that despite ongoing research, still there is no concrete parameter(s) of vascular dysregulation, which would be easily measurable, therapeutically influenceable as directly as possible, and predictive in terms of future glaucomatous damage.
Rapidly developing technologies such as OCT-A may be more predictive of future glaucoma damage by virtue of combining functional and morphological information. But we are far away from prime time.

Systemic and ocular risk factors in normal tension glaucoma

Swedish Glaucoma Society Annual Meeting

Sustained drug delivery systems: do they make a difference?

Sustainable effective treatment options
Dr. Tony Realini discussed what sustainable effective treatment options are, highlighting the limitations of each option in the low-income population setting. One promising option discussed is the SLT with its safety profile. Efficacy data from a low-income environment is presented.

Surgical Therapy

Surgical Techniques and implantation sites

Surgical technique and its modifications

Surgical technique and Effectiveness of low cost glaucoma drainage device

Surgical solution for post LASIK secondary glaucoma

Surgical outcomes and vision

Surgical Outcome of Childhood Glaucoma Surgery in Sudan

Surgical Nightmares

Surgical management of POAG: Bangladesh scenario

Surgical management of nanophthalmos with angle-closure glaucoma | Sharmila Rajendrababu
Nanophthalmos is a rare disease with crowded anterior segment and increased scleral thickness.
Surgery in Nanophthalmos is often prone for Vision threating complications like Uveal effusions and retinal detachment. Careful pre-operative planning and intraoperative Prophylactic Selerostomy may minimize the risk of complications.
This presentation is meant to provide an overview and practical tips for safe surgical management in short eyes.

Surgical Grand Rounds | Registration
Surgical Grand Rounds | Post webinar feedback survey
Surgical Grand Rounds | Live Chat
Surgical Grand Rounds | Live Chat
Joining the live chat is the best way to get involved during the WGA Surgical Grands Rounds webinar: connecting with other attendees and asking questions. We’ll be live via YouTube, so you’ll need to log in with a Google account or set up a new account to join the live chat.
You’ll be able to view the broadcast without logging in to your Google account, but you’ll be unable to chat. While it does take a few steps to chat, we are confident this opportunity to connect with the global glaucoma community enhances the free WGA Surgical Grand Rounds.
Here’s a step-by-step guide for joining the conversation:
How to join the live chat
I have a Google account. What do I do?
You’re in luck! All you need to do is head to the WGA Surgical Grand Rounds broadcast page and sign in to your Google account. If you haven’t used YouTube with your Google account before, you’ll need to “create a channel”. Once you’re logged in, YouTube will ask you to create a channel to join a live chat if you haven’t done so previously. Check out our instructions below for creating a channel with your Google account.
I don’t have a Google account. What do I do?
First, you’ll need to create a Google account. Check out their step-by-step guide here to create your account and prepare you for the next step. You don’t need to set up a Gmail account to have a Google account! Here’s a helpful tip from Google Account Help:
“Tip: You don’t need a Gmail account to create a Google Account. You can use your non-Gmail email address to create one instead.”
I’m logged in, but I need to create a channel. What do I do?
In order to participate in YouTube live chat, you’ll need to “create a channel” associated with your Google account. Here’s what you’ll need to do:
- Head to the WGA Surgical Grand Rounds broadcast page
- In the chatbox, click on the “Create a Channel to Join the Chat” button.
- Enter the First Name and Last Name of how you’d like to appear in the live chat.
- You’re ready to chat! Be sure to log in to the same Google account during the broadcast.
Questions? Reach out to the WGA Executive Office via info@worldglaucoma.org.
Surgical Grand Rounds – Registration Confirmation
Surgical Grand Rounds
About the Surgical Grand Rounds
In 2022 the WGA launched a new webinar series, focused on surgical challenges that glaucoma specialists are likely to face: WGA Surgical Grand Rounds. Each webinar features two scenarios of surgical challenges or complications. After each presentation, the speaker joins an expert panel for a brief discussion and answers questions related to the presentation. Get ready for state-of-the-art surgery videos and discussions from the world’s most skilful glaucoma surgeons!
7th WGA Surgical Grand Rounds Webinar has wrapped up – January 29, 2026
- GATT – Current Technique, Preventing and Managing Complications
- Presented by Davinder Grover, MD (United States)
- Moderated by Tanuj Dada, MD (India)
- Panelists: Xiulan Zhang, MD (China) & Devendra Maheshwari, MD (India)
- Correct Technique I Stent/ Hydrus, Preventing and Managing Complications
- Presented by Paul Harasymowycz, MD (Canada)
- Moderated by Pradeep Ramulu, MD (United States)
- Panelists: Chelvin Sng, MD (Singapore) & Paul Healey, MD (Australia).
If you missed it, don’t worry — the on‑demand recording will be available in the coming weeks. Sign up for our Newsletter to be notified as soon as it’s published.
Industry Support
We would like to recognise the ancillary support of our Industry partners in bringing the 7th edition of WGA’s Surgical Grand Rounds webinar to life.
Previous Editions
6th edition of Surgical Grand Rounds – September 19, 2024
- Avoiding/managing the infected bleb post Trabeculectomy presented by Vivek Dave, MD (India). Panelists: Winnifred Nolan, MD (United Kingdom) and Kuldev Singh, MD (United States). Moderated by Tanuj Dada, MD (India).
- Avoiding/managing infections after subconjunctival implants (XEN/Preserflo/Long tubes) presented by Davinder Grover, MD (United States). Panelists: Kaweh Mansouri, MD (Switzerland) and Jennifer Fan Gaskin, MD (Australia). Moderated by Pradeep Ramulu, MD (United States).
5th edition of Surgical Grand Rounds – November 30, 2023
- Choroidal Detachment presented by Sameh Mosaed, MD (United States). Panelists: Liza Sharmini, MD (Malaysia) and Catherine Jiu-Ling Liu, MD (Taiwan). Moderated by Pradeep Ramulu, MD (United States).
- Suprachoroidal Hemorrhage after Glaucoma Surgery presented by Saurabh Verma, MD (India). Panelists: Christina Weng, MD (United States) and Paul Healey, MD (Australia). Moderated by Tanuj Dada, MD (India).
4th edition of Surgical Grand Rounds – January 26, 2023
- How to Manage Failing/Failed Filter presented by Andrew Tatham, MD (United Kingdom). Panelists: Sirisha Senthil, MD (India) and Michael Coote, MD (Australia). Moderated by Tanuj Dada, MD (India).
- Tube Revisions to Restore Flow presented by Leon Herndon, MD (United States). Panelists: Joseph Anthony Tumbocon, MD (Philippines) and Ying Han, MD (United States). Moderated by Pradeep Ramulu, MD (United States).
3rd edition of Surgical Grand Rounds – July 7, 2022
- Malignant Glaucoma presented by Leon Au, MD (United Kingdom). Panelists: Harry Quigley, MD (United States) and Esther Hoffmann, MD (Germany). Moderated by Tanuj Dada, MD (India).
- Nanophthalmos with Glaucoma presented by Shamira Perera, MD (Singapore). Panelists: Sharmila Baburajendran, MD (India) and Mohammed Pakravan, MD (United States). Moderated by Pradeep Ramulu, MD (United States).
2nd edition of Surgical Grand Rounds – April 14, 2022
- Managing hypotony after trabeculectomy presented by Vijaya Lingham, MD (India). Panelists: Vital Costa, MD (Brazil) and Paul Healey, MD (Australia). Moderated by Tanuj Dada, MD (India).
- Managing hypotony after tubes presented by Keith Barton, MD (United Kingdom). Panelists: Steve Gedde, MD (United States) and Anne Coleman, MD (United States). Moderated by Pradeep Ramulu, MD (United States).
1st edition of Surgical Grand Rounds – January 27, 2022
- Treatment of bleb dysesthesia/overhanging blebs presented by Paul Palmberg, MD (United Staets). Panelists: Yvonne Buys, MD (Canada) and Peng Khaw, MD (United Kingdom). Moderated by Tanuj Dada, MD (India).
- Pseudoexfoliation glaucoma with small pupil and cataract with zonular weakness presented by Arsham Sheybani, MD (United States). Panelists: Antonio Fea, MD (Italy) and Marlene Moster, MD (United States). Moderated by Pradeep Ramulu, MD (United States).
Surgical game changers: what’s beyond MIGS?
Dr. Ike Ahmed closes the symposium discussing how being Proactive vs Reactive can influence outcomes in glaucoma surgery. He starts by discussing the rates of progression and blindness in the real world and their possible reasons. He suggests it is now time to change the treatment paradigm in glaucoma by being more aggressive from the start and aiming for lower pressure targets. He ends his talk by proposing minimally invasive procedures and new drug delivery systems as tools to overcome issues with adherence to medical therapy.

Surgical complications in myopic patients
We need to consider the unique traits of myopic eyes before surgical intervention for glaucoma and to choose safer and more conservative approaches, such as MIGS, NPGS, etc.
It is important to avoid large intraoperative or postoperative IOP fluctuations in cases where trabeculectomy is performed.
In cases with postoperative hypotony, early intervention must be done to prevent vision loss due to hypotony maculopathy.
From the Education Committee
Dr. Ricardo Guedes talked about the need to consider the unique traits of myopic eyes before surgical intervention for glaucoma and to choose safer and more conservative approaches, such as MIGS, NPGS, etc. He highlighted that large intraoperative or postoperative IOP fluctuations must be avoided in cases where trabeculectomy is performed. In cases with postoperative hypotony, early intervention must be done to prevent vision loss due to hypotony maculopathy.

Surgical approaches to acute angle closure
Dr. Rojanapongpun discussed the fundamental concepts, approaches and procedures in the surgical management of acute angle closure. He said that angle closure is a surgical disease because surgical approaches are needed to address the angle closure mechanisms. He mentioned that the success of surgical approach in angle closure depends on the stage of angle closure (PACS, PAC or PACG) and the mechanism of angle closure (pupillary or non-pupillary block). He also spoke on the pros and cons of different laser and surgical procedures in the management of acute angle closure.

Surgical approaches and unique considerations in africa
Dr. Dan Kiage discussed the surgical approach and the unique considerations in Africa separately for each of the glaucoma surgical procedures.

Surgical Approaches and Unique Considerations

Surgical approach to glaucoma in Sri Lanka

Surgery, not medicine, should be the standard firstline treatment for open-angle glaucoma in SSA

Surgery in juvenenile uveitic glaucoma
Surgery is usually required with peri-operative management of inflammation; drainage procedures significant risk of hypotony ; goniotomy – potentially successful, low complication rates; trabeculectomy – potentially more complications especially hypotony; glaucoma drainage devices – successful ?? limited aqueous production, significant complications especially hypotony, consider smaller surface area implant
and avoid cyclodestruction procedures.

Surgery and aqueous humor dynamics

Surgery after a failed trabeculectomy

Supraciliary Shunts/ Implants

Suprachoroidal Surgery with Miniject
The film shows original footage of a cataract extraction in the year 1925 at the Medical University of Graz in the first part. In the second part the implantation of a Miniject is shown and explained.
Ewald Lindner Medical University of Graz

Suprachoroidal space in the pathogenesis of glaucoma – morphological and biomechanical analysis

Suprachoroidal hemorrhage

Suprachoroidal Hemorrhage

Suprachoroidal drainage

Suprachoroidal devices
Several procedures have been proposed to reduce IOP using the suprachoroidal space. Although interesting, in the past, all the attempts failed. The video presents a new device that may offer advantages and avoid some of the complications encountered in the past.
From the Education Committee
Suprachoroidal devices were next presented by Dr. Antionio Fea, highlighting their advantages and limitations, including the Cypass that was removed from the market. The advantages and limitations of the suprachoroidal space for filtration is discussed, and novel devices, some not commercially available yet, presented.

Supporting glaucoma patients through support networks

Support files overview
WGA#One is your gateway to the World Glaucoma Association. With a WGA#One account you can access knowledge resources and join our community.
Create a free WGA#One account to join the largest international glaucoma network.
If you need assistance, please contact the WGA Executive Office at
info@worldglaucoma.org
Login
Summary and Concluding Remarks

Sulcus Tube placement

Sudden visual scotoma in a woman with exfoliation glaucoma
What may explain the sudden appearance of central scotoma in one eye with pseudo-exfoliation and ocular hypertension after pupillary dilation? This case presentation, by Luis Silva, will bring you one possible explanation. Watch the video and learn more about paracentral acute middle maculopathy (PAMM).

Suconjunctival Outflow and Bleb Biology

Subscribe to Newsletter
Our newsletters are managed through WGA#One, which is the name of our online data management system.
WGA#One will give you full access to exclusive WGA content, such as the IGR or Educational Portal. It will also provide you with the opportunity to directly, at any given moment, change personal details such as your email address.
Please click on the appropriate link below to navigate to the newsletter subscription form.
Medical Professional Newsletter Subscription Form
Industry Professional Newsletter Subscription Form
Glaucoma Patient Newsletter Subscription Form
Newsletter Archive
2021
- Read the latest Journal of Glaucoma – Vol. 30, No. 6, June 2021
- Your WGA update for May
- Reminder: The 5th WGA Global Webinar starts soon!
- [5th WGA Webinar] Speaker line-up
- Read the latest Journal of Glaucoma – Vol. 30, No. 5, May 2021
- [5th WGA Webinar] The program is here
- 🎥 Watch the April WGA Paper of the Month video from the Journal of Glaucoma!
- Your WGA update for April
- Join us for the 5th Global Webinar on Glaucoma
- Reminder: The 4th WGA Global Webinar starts soon!
- 🎥 Watch the March WGA Paper of the Month video from the Journal of Glaucoma!
- [4th WGA Webinar] Speaker line-up
- [4th WGA Webinar] The agenda is here
- Your WGA update for March
- Join us for the 4th Global Webinar on Glaucoma
- That’s a wrap on World Glaucoma Week!
- World Glaucoma Week starts today!
- 🎥 Watch the JOG Paper of the Month February video!
- Only 1 week to World Glaucoma Week
- Your WGA update for February
- Countdown to World Glaucoma Week
- Get ready for World Glaucoma Week
- Reminder: the 3rd WGA Global Webinar starts soon!
- Speaker line-up for the 3rd Global Webinar on Glaucoma
- 🎥 Watch the JoG Paper of the Month January video!
- The agenda of the 3rd WGA Global Webinar
- Your WGA update for January
- 👉 You are invited to the 3rd Global Webinar on Glaucoma
- 🎥 Watch the JoG Paper of the Month December video!
2020
- ✨ Happy New Year! ✨
- Your WGA update for December
- Reminder: the 2nd Global Webinar on Glaucoma starts soon!
- Speaker line-up for the 2nd Global Webinar on Glaucoma
- 🎥 Watch the JoG Paper of the Month November video!
- The agenda of the 2nd Global Webinar on Glaucoma
- Your WGA update for November
- 💻 Join us for the 2nd Global Webinar on Glaucoma
- 🎥 Watch the JoG Paper of the Month October video!
- Online now: the Global Webinar on Glaucoma Surgery recording
- Your WGA update for October
- Only 1 day to go
- Your local time for the WGA Global Webinar
- This Saturday: Global Webinar on Glaucoma Surgery
- Don’t miss the Glaucoma Surgery webinar
- 🎥 Watch the JoG Paper of the Month September video!
- 💻Free Glaucoma Surgery webinar this Saturday
- Your WGA update for September
- Coming soon: a new WGA initiative!
- 🎥 Watch the JoG Paper of the Month July video!
- Easier access to the WGA Online Courses
- Your WGA Update for July
- 🎥 Watch the JoG Paper of the Month June video!
- Your WGA Update for June
- WGC-2021 | New dates!
- Meet us at WOC2020 Virtual®
- 🎥 Watch the JoG Paper of the Month May video!
- Your WGA Update for May
- WGC-2021 message by the Executive Committee of the WGA
- 🎥 Watch the JoG Paper of the Month video!
- Your latest WGA Update
- Ophthalmology and Glaucoma Practice in the COVID-19 Era
- Your WGA Update for March
- 🔜 Countdown to #glaucomaweek
- Your WGA Update for February
- Green = Go #glaucomaweek
- Get ready for World Glaucoma Week 2020
- World Glaucoma Week 2020: Save the date
- Your WGA Update for January
2019
- Happy New Year!
- Your WGA Update for December
- Your latest WGA Update
- Your WGA Update for October
- Quicker access to the Journal of Glaucoma for free
- Your latest WGA Update – fall 2019
- Your latest WGA Update – summer 2019
- Join the “Meet the Glaucoma Expert” webinar
- Your WGA Update for April
- World Glaucoma Week off to a great start!
- Only 1 week to World Glaucoma Week 2019
- Your WGA Update for February
- Countdown to World Glaucoma Week 2019
- 12 hours left to save!
- More time to save: extended deadline WGC-2019
- World Glaucoma Week 2019: Plan & Prepare
- WGC-2019: last chance to save
- Your WGA Update for January
- Save up to AUD$ 250 on registration fees
- Book your wetlab at WGC-2019 now
Subliminal cyclophotocoagulation in neovascular glaucoma

Subconjunctival Outflow MIGS

Subconjunctival MIGS

Subconjunctival drainage implants – Ab interno is the preferred approach

Subconjunctival drainage implants – Ab Externo is better than Ab interno

Subconjunctival drainage implants

Subconjunctival drainage implants

Subconjunctival Delivery of Stanniocalcin-1 via Adenoassociated Virus Provides Sustained Intraocular Pressure Reduction

Subconj MIGS (Xen & Preserflo)

Structure: How to determine glaucoma progression by OCT / HRT
Linda Zangwill gave insights on detecting progression by the OCT. She mentioned how recent advances in OCT technology have enabled OCT angiography, measurement of the Bruchs membrane opening and Ganglion cell complex have provided much more clinical information challenges still exist in terms of little information regarding age-related change. However deciding what rate of change is clinically meaningful on the OCT can be challenging. She emphasized that using automated progression analysis is central to judging progression.

Structure/function relationship according to disease severity: how to merge these information into clinical decision making process
Felipe Mediros spoke on how clinical implications of the structure function relationship and clinical disease severity. He mentioned that in general OCT detected change in early disease and perimetry in later disease. He described the combined structure function index that can be used merge information from both sources.

Structure-function relationship in the temporal raphe region
The temporal raphe is often deviated from the horizontal meridian. The structural temporal raphe is more deviated to the perimetrically normal hemiretina side than the functional temporal raphe in glaucomatous eyes with a hemifield defect.
Structural change may precede a functional loss at the temporal raphe region in glaucomatous eyes.

Structure function relationship
Kouros Nouros Mahdavi gave an excellent talk on structure-function relationship. He said it provided complementary information and helped in the confirmation of disease or progression and also helped in prediction of disease. He compared OCT and SAP and gave several reasons why structure and function may disagree. He mentioned that glaucoma severity influences structure and function relationship and that inter individual variability was more than intra eye variability. He said that customization could improve structure function relationship. All structural parameters have a measurement floor because of the blood vessel glial tissue and the remaining connective tissue in the retina. He added that structural measurements can predict functional progression. He concluded by saying that structure and function can be unified into a single index and longitudinal Structure Function relationship can help with determination of progression.

Structure and Function: Can AI optimize Visual Function assessment from Imaging data?

Steroid induced Glaucoma

Step-wise procedure in glaucoma management

Stenting procedures

Stem cells for the the modelling of glaucoma in a dish

Statutes Committee Nomination Form
Statutes Committee
Stand-alone Trabecular MIGS: should we always consider SLT first? YES

Stand-alone Trabecular MIGS: should we always consider SLT first? NO

SRG 2019
12th Congress of the Romanian Society of Glaucoma
Spotlight on Africa

Soft eyes

Society Symposium WGC-2021
It is no longer possible to submit your request.
Please contact Marije de Graaf at info@worldglaucoma.org, should you have any questions.
Society Spotlight | Zambia Glaucoma Interest Group

Society Spotlight | Vietnam Glaucoma Club

Society Spotlight | Venezuelan Glaucoma Group

Society Spotlight | Uruguayan Glaucoma Society

Society Spotlight | United Kingdom and Éire Glaucoma Society

Society Spotlight | Ukrainian Glaucoma Society

Society Spotlight | Thai Glaucoma Society

Society Spotlight | Swedish Glaucoma Society

Society Spotlight | Sudanese Glaucoma Association

Society Spotlight | Spanish Glaucoma Society

Society Spotlight | South African Glaucoma Society

Society Spotlight | Slovak Glaucoma Society

Society Spotlight | Serbian Glaucoma Society

Society Spotlight | Saudi Glaucoma Group

Society Spotlight | Salvadoran Glaucoma Society

Society Spotlight | Russian Glaucoma Society

Society Spotlight | Romanian Glaucoma Society

Society Spotlight | Puerto Rican Glaucoma Society

Society Spotlight | Portuguese Glaucoma Group

Society Spotlight | photo upload
It is no longer possible to upload additional photos.
You may share your additional photos by email.
Society Spotlight | Philippine Glaucoma Society

Society Spotlight | Peruvian Glaucoma Society

Society Spotlight | Paraguayan Glaucoma Society

Society Spotlight | Pan American Glaucoma Society

Society Spotlight | Pakistan Glaucoma Association

Society Spotlight | Optometric Glaucoma Society

Society Spotlight | Norwegian Glaucoma Society

Society Spotlight | Netherlands Glaucoma Group

Society Spotlight | Moroccan Glaucoma Society

Society Spotlight | Middle East Africa Glaucoma Society

Society Spotlight | Mexican Glaucoma Society

Society Spotlight | Malaysian Glaucoma Society

Society Spotlight | Lithuanian Glaucoma Society

Society Spotlight | Lebanese Glaucoma Society

Society Spotlight | Latin American Glaucoma Society

Society Spotlight | Korean Glaucoma Society

Society Spotlight | Japan Glaucoma Society

Society Spotlight | Italian Association for the Study of Glaucoma

Society Spotlight | Israel Glaucoma Group

Society Spotlight | Iranian Glaucoma Society

Society Spotlight | International Society of Glaucoma Surgery

Society Spotlight | Indonesian Glaucoma Society

Society Spotlight | Guatemalan Glaucoma Society

Society Spotlight | Greek Glaucoma Society

Society Spotlight | Glaucoma Society of the Turkish Ophthalmology Association

Society Spotlight | Glaucoma Society of the Taiwan Academy of Ophthalmology

Society Spotlight | Glaucoma Society of the German Ophthalmological Society

Society Spotlight | Glaucoma Society of the Croatian Ophthalmological and Optometric Society

Society Spotlight | Glaucoma Society of Panama

Society Spotlight | Glaucoma Society of Nigeria

Society Spotlight | Glaucoma Society of Nepal

Society Spotlight | Glaucoma Society of India

Society Spotlight | Glaucoma Society of Ecuador

Society Spotlight | Glaucoma Society of Colombia

Society Spotlight | Glaucoma Society of Chile

Society Spotlight | Glaucoma Section of the Polish Society of Ophthalmology

Society Spotlight | Glaucoma Section of the Hungarian Ophthalmological Society

Society Spotlight | Glaucoma Organization of the Austrian Ophthalmological Society

Society Spotlight | Glaucoma Interest Group of the Myanmar Ophthalmological Society

Society Spotlight | Glaucoma Interest Group of the College of Ophthalmologists of Sri Lanka

Society Spotlight | Glaucoma Group of the Swiss Society of Ophthalmology

Society Spotlight | Glaucoma Group of the Slovenian Society of Ophthalmology